Inpatient
We require authorization or pre-approval for inpatient requests for cancer treatment services for all members. Notification to Blue Cross is required. Go to our Prior Authorization Overview page for tips for submitting authorization requests.
For FEP members, please check authorization requirements at fepblue.org.Outpatient
Commercial and Medicare Advantage members
We require prior authorization for certain outpatient medical oncology and radiation oncology services through our Quality Care Cancer Program. The program is administered by Carelon Medical Benefits Management, an independent company, so authorization requests should go directly to them.
Note: Indemnity members are not part of the Quality Care Cancer Program.
Outpatient medical oncology services and supportive care medications as noted in our medical policies:
- Quality Care Cancer Program (Medical Oncology) (099)
- Supportive Care Treatments for Patients with Cancer (105)
Radiation oncology services as noted in our medical policies:
Ordering providers will request authorization with Carelon in one of three ways:
- Through a direct link on this site (no additional registration is required). In the eTools tab, go to Carelon. Click the Go Now button.
- Go directly to the Carelon ProviderPortal (registration is required) at www.providerportal.com.
Note: If you’ve already registered for the Carelon ProviderPortal for Blue Cross Blue Shield of Massachusetts or another insurer, you won’t need to register again. - Call Carelon’s Contact Center at 1-866-745-1783
- Available Monday through Friday, 8 a.m. – 6 p.m. If you leave a voicemail after these hours, Carelon will respond the next business day.
Required information:
- Member first, last name and date of birth
- Ordering provider’s first and last name
- Dispensing provider name
- Place of service
Most order request also may require:
- Clinical details
- Patient height and weight
- Diagnosis
- Cancer type
- Pathology and stage
- Chemotherapy regimen
- Biomarkers and tumor characteristics
- Line of treatment
For order entry worksheets and checklists, click here.
Required information:
- Member first, last name and date of birth
- Ordering provider’s first and last name
- Primary cancer treatment being requested (for example, brachytherapy, IMRT, proton beam, etc.)
- Patient diagnosis
- Name and location of facility where treatment will be administered
Clinical data required:
- Pre-Exam Questions (PEQ):
- Patient’s height and weight
- T, N, M status or stage of cancer
- Cancer histology
- Performance status, either Karnofsky or ECOG
- Treatment goal, total dose, and number of fractions
- For some situations, plan comparison with 3D or IMRT is required. This information is available on Carelon’s radiation therapy website.
After entering and reviewing your request, you’ll receive a summary. Approved orders will indicate “Authorized” and will include an “Order ID.” You’ll also see a summary of codes and disease information.
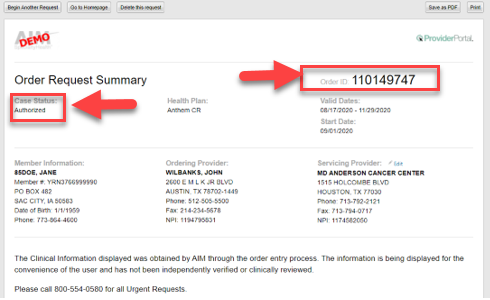
To avoid a denied claim, servicing providers should use the Carelon's ProviderPortal to verify that an authorization is in place before the service is performed.
- March 1, 2021 News Alert for some provider types, "Outpatient cancer care requires authorization starting July 1" (Only viewable to some provider types.)
- Carelon’s medical oncology website for Blue Cross Blue Shield of Massachusetts
- Carelon’s radiation therapy website
- Carelon’s radiation oncology clinical guidelines
![]() S-code Fact Sheet (log in required )
S-code Fact Sheet (log in required )
- March 1, 2021 News Alert, "Outpatient cancer care requires authorization starting July 1" () Only viewable to some provider types.
- Carelon’s medical oncology website for Blue Cross Blue Shield of Massachusetts
- Carelon’s radiation therapy website
- Carelon’s radiation oncology clinical guidelines
Federal Employee Program members
Federal Employee Program (FEP) members are not included in the Quality Care Cancer Program, but they may have authorization or pre-certification requirements for their outpatient cancer services. To check authorization requirements, please visit fepblue.org.


