Before performing a service, you should:
| Step |
Check a member’s eligibility and benefits, including authorization requirements.
Use an eTool like ConnectCenter. The eTool Authorization Manager can be used to verify eligibility but does not provide benefit information. |
| Step |
If necessary, request authorization. For most situations, the fastest way to request authorization is to use Authorization Manager.
|
Authorization is not required for psychotherapy, psychiatric office visits, or mobile crisis intervention.
In addition, if a POS member is using their out-of-network benefits, authorization requirements do not apply.
Authorization and medical necessity resources
| To | Then |
|---|---|
|
Refer to medical policies for Federal Employee Program members and Commercial HMO/POS and PPO members.
For Medicare Advantage members, begin with medical policy 132, Medicare Advantage Management. When there is no applicable Coverage Determination (NCD or LCD*), we follow our commercial medical policies. |
|
Download our Authorization Quick Tip and go to the page titled Mental health authorization notification requirements. |
|
Read our medical policy document, Clinical Exception Process (Individual Consideration). |
* For Medicare Advantage members, we are required to make coverage determinations for services through the CMS National Coverage Determination (NCD) policies and benefit manuals. In addition, we follow Local Coverage Determination (LCD) policies established by the Massachusetts Medicare Administrative Contractors. These policies supersede our commercial medical policies.
Federal Employee Program (FEP) resources
FEP frequently has its own requirements. Detailed benefit descriptions, including exclusions and member copayment information for these services, are available in the Blue Cross and Blue Shield Service Benefit Plan brochures.
Acute care and intermediate services
For most plans, we require notification (not prior authorization) within 72 hours of admission for the initial 72 hours.
The facility must call the number on the back of the member’s ID card to notify us of the admission. If the member does not have their ID card, call 1-800-524-4010.
- “precertification” is the review of inpatient hospital stays to ensure they’re medically necessary before you receive services, and
- “prior approval” is the review of specific services or prescription drugs to ensure they are medically necessary.
Precertification is required for acute inpatient care. If we don’t receive precertification within 48 hours of the admission, the member will have to pay a $500 penalty. To request precertification:
- Call 1-800-524-4010.
- Fax the Behavioral Health - Level of Care Request Form to us at the number listed on the cover sheet.
Note: FEP members with the Basic Option or FEP Blue Focus plan can only use providers who participate in our PPO networks.
Intermediate services may include acute residential treatment (sub-acute care), partial hospitalization programs, intensive community-based treatments (for children and adolescents), and intensive outpatient programs.
All authorizations for intermediate services are based on the medical necessity of services.
| Plan type | Admission type | Requirement |
|---|---|---|
| Commercial HMO/POS and PPO | Mental health | Notification within 72 hours of admission. |
| Commercial HMO/POS and PPO | Substance use | Notification within 48 hours of admission (for adults) or 72 hours of admission (for children and adolescents 22 years of age or less). |
| Medicare Advantage | Either mental health or substance use | Prior authorization is required. |
| Federal Employee Program | Either mental health or substance use | Precertification is required, and additional requirements apply. See below. |
The member must be enrolled in case management before the facility can request precertification. To enroll, providers (or members themselves) can refer the member for residential treatment by calling FEP Case Management Program at 1-800-689-7219 ext. 31133.
If a member does not receive precertification before being admitted, benefits will not be covered for their services.
Facilities should call FEP at 1-800-524-4010 before the admission. You will need to provide:
- The member’s written consent for participation in case management, and
- A preliminary treatment and discharge plan.
- Authorization is required for Medicare Advantage and Commercial HMO/POS and PPO plans.
- No precertification is required for FEP.
- When covered, prior authorization is required. Check benefits and eligibility before rendering services.
- Not a covered benefit for FEP, and not typically a benefit for Medicare Advantage.
![]() Behavioral Health for Children and Adolescents Fact Sheet (for community mental health centers)
Behavioral Health for Children and Adolescents Fact Sheet (for community mental health centers)
If you have questions, you can call Behavioral Health Clinical Intake at 1-800-524-4010.
Fax numbers are in the “Contact Us” section of our Prior Authorization Overview page.
Inpatient
We require authorization or pre-approval for inpatient requests for cancer treatment services for all members. Notification to Blue Cross is required. Go to our Prior Authorization Overview page for tips for submitting authorization requests.
For FEP members, please check authorization requirements at fepblue.org.Outpatient
Commercial and Medicare Advantage members
We require prior authorization for certain outpatient medical oncology and radiation oncology services through our Quality Care Cancer Program. The program is administered by Carelon Medical Benefits Management (formerly AIM Specialty Health), an independent company, so authorization requests should go directly to them.
Note: Indemnity members are not part of the Quality Care Cancer Program.
Outpatient medical oncology services and supportive care medications as noted in our medical policies:
- Quality Care Cancer Program (Medical Oncology) (099)
- Supportive Care Treatments for Patients with Cancer (105)
Radiation oncology services as noted in our medical policies:
Ordering providers will request authorization with Carelon in one of three ways:
- Through a direct link on this site (no additional registration is required). In the eTools tab, go to Carelon. Click the Go Now button.
- Go directly to the Carelon ProviderPortal (registration is required) at www.providerportal.com.
Note: If you’ve already registered for the Carelon ProviderPortal for Blue Cross Blue Shield of Massachusetts or another insurer, you won’t need to register again. - Call Carelon’s Contact Center at 1-866-745-1783
- Available Monday through Friday, 8 a.m. – 6 p.m. If you leave a voicemail after these hours, Carelon will respond the next business day.
Required information:
- Member first, last name and date of birth
- Ordering provider’s first and last name
- Dispensing provider name
- Place of service
Most order request also may require:
- Clinical details
- Patient height and weight
- Diagnosis
- Cancer type
- Pathology and stage
- Chemotherapy regimen
- Biomarkers and tumor characteristics
- Line of treatment
For order entry worksheets and checklists, click here.
Required information:
- Member first, last name and date of birth
- Ordering provider’s first and last name
- Primary cancer treatment being requested (for example, brachytherapy, IMRT, proton beam, etc.)
- Patient diagnosis
- Name and location of facility where treatment will be administered
Clinical data required:
- Pre-Exam Questions (PEQ):
- Patient’s height and weight
- T, N, M status or stage of cancer
- Cancer histology
- Performance status, either Karnofsky or ECOG
- Treatment goal, total dose, and number of fractions
- For some situations, plan comparison with 3D or IMRT is required. This information is available on Carelon’s radiation therapy website.
After entering and reviewing your request, you’ll receive a summary. Approved orders will indicate “Authorized” and will include an “Order ID.” You’ll also see a summary of codes and disease information.
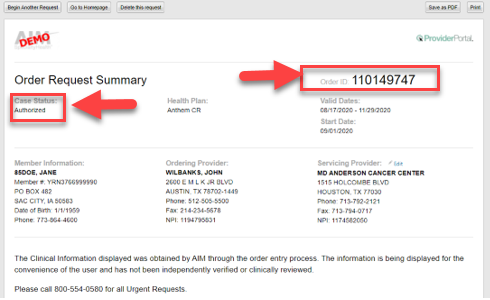
To avoid a denied claim, servicing providers should use the Carelon's ProviderPortal to verify that an authorization is in place before the service is performed.
- March 1, 2021 News Alert for some provider types, "Outpatient cancer care requires authorization starting July 1" (Only viewable to some provider types.)
- Carelon’s medical oncology website for Blue Cross Blue Shield of Massachusetts
- Carelon’s radiation therapy website
- Carelon’s radiation oncology clinical guidelines
![]() S-code Fact Sheet (log in required )
S-code Fact Sheet (log in required )
- March 1, 2021 News Alert, "Outpatient cancer care requires authorization starting July 1" () Only viewable to some provider types.
- Carelon’s medical oncology website for Blue Cross Blue Shield of Massachusetts
- Carelon’s radiation therapy website
- Carelon’s radiation oncology clinical guidelines
Federal Employee Program members
Federal Employee Program (FEP) members are not included in the Quality Care Cancer Program, but they may have authorization or pre-certification requirements for their outpatient cancer services. To check authorization requirements, please visit fepblue.org.
Care management programs we offer help address members who are:
- Seriously ill or have complex conditions
- Managing a chronic condition
- At risk for developing serious or chronic illnesses
- Recently hospitalized and could benefit from after care or transitions in care support
We identify members based on multiple sources, including medical and pharmacy claims, and other self-reported information.
Interventions are designed to help members avoid illness, boost wellness, enhance quality outcomes, and decrease health care costs by addressing gaps in care and medication management in accordance with their clinician’s or physician’s treatment plan. These interventions may include:
- Educational and informational materials to help members understand and manage their medications, make appropriate lifestyle choices, and find additional resources for support
- Ways to plan for effective doctor visits
- Preventive screening and lab reminders
- Review of medications to address any potential safety issues, adherence, or other reminders
- Reviewing social determinants of health, such as food insecurity and financial issues, and offering support to help address those needs
- Case management and navigation support after a hospitalization
Some members receive additional nurse coaching by phone. We reach out to treating providers if there are specific concerns raised that you may need to be aware of.
We welcome provider and member referrals. If you think a member could benefit from care management, please complete our Patient Referral for Health Management Programs & Services Form and return it to the fax number indicated. Or, call Health Management Programs at 1-800-392-0098, Option 1.
For questions about Federal Employee Program member referrals, please call 1-800-689-7219, Option 2.
| For members with this plan | Call |
|---|---|
| HMO, PPO, Indemnity | Case Management 1-800-392-0098, Option 1 |
| Federal Employee Program (FEP) | FEP Case Management 1-800-689-7219, Option 2 |
| Medicare Advantage | Case Management MedAdvCMreferrals@bcbsma.com 1-800-392-0098, Option 1 |
| Medex | Case Management 1-800-392-0098, Option 3 |
Chiropractors should request authorization for chiropractic services for certain Blue Cross Blue Shield of Massachusetts members. WholeHealth Living, Inc., a Tivity Health Company, administers the program
Many, but not all, members in these plans need an authorization for chiropractic services. Please check benefits and eligibility to determine if authorization is required.
| Plan name | Additional information |
|---|---|
| HMO/POS plans | |
| HMO Blue Blue Choice Plan 2 Network Blue |
If the member has a 12 visit limit to their chiropractic benefits, authorization doesn't apply. |
| HMO/POS New England Plans (some account exclusions apply) | |
| Access Blue New England HMO Blue New England Network Blue® New England Blue Choice® New England (POS) Blue Choice® New England Plan 2 (POS) |
Includes members who:
|
Use ConnectCenter to see if the member requires authorization.
Go to Verification>New Eligibility Inquiry and complete required fields. Click Submit.
Scroll to view the response. Under Eligibility, look for Chiropractic. Authorization information appears in the fields under Message and Auth/Cert Required. If authorization is required, you'll see a message indicating the authorization is required for visits 13 and beyond.
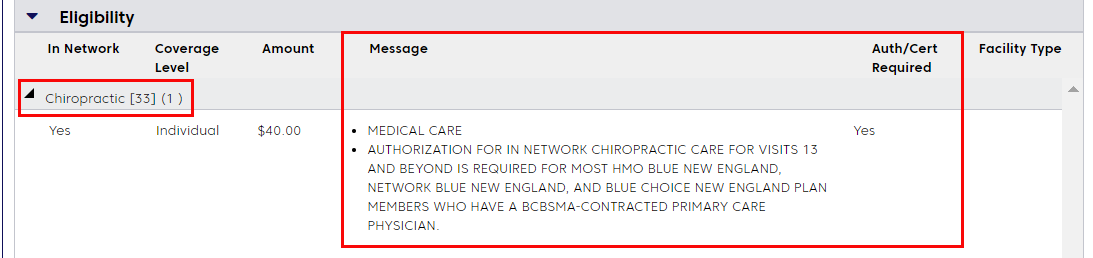
If authorization is not required, you'll see a message like the one below. This message may appear if the member has a 12 visit benefit limit for chiropractic services.
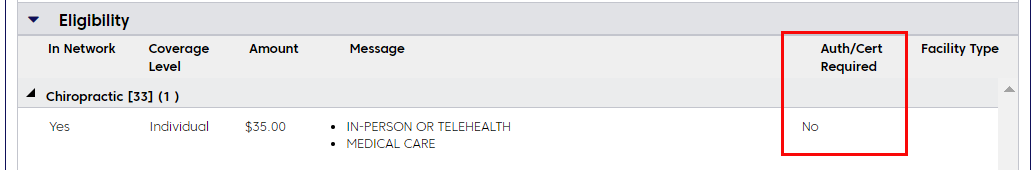
Request authorization before the member's 13th visit. You can do this using WholeHealth Living’s web-based Rapid Response System.
Authorization requests must be submitted within seven days (+/-) from the date of the member’s 13th visit.
It’s helpful to have the following information ready to enter into the Rapid Response System (web or phone-based).
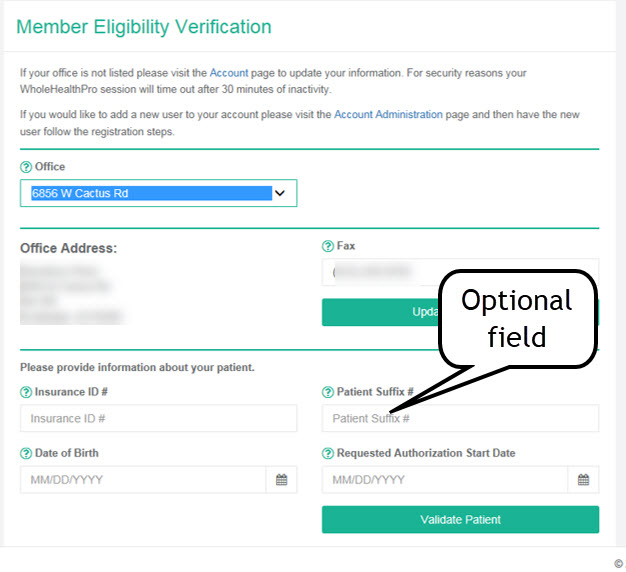
- The member’s ID number (prefix and suffix are not required) and date of birth.
- The injury mechanism (auto accident or work-related injury) or the presence of other insurance (if the other health insurance is primary and coordination of benefits applies).
- The member’s score from the Patient-specific Functional Scale (leave blank if member refuses to answer questions). The Patient-specific Functional Scale is available in English, Spanish, and Portuguese.
- Primary, secondary, and/or tertiary diagnosis codes.
You should also have the member’s medical record available since you will be asked multiple questions about the member’s diagnosis(es), medical history, and treatment plan.
Please refer to the Chiropractic Care Plan Authorization Request Form in the Appendix of the Chiropractic Services Authorization Program Guide for a complete list of the questions you will be asked to enter into the RRS.
- Web browser compatibility: Works best with Internet Explorer 11.
- Communication preferences: To get messages from WholeHealth Living’s about your authorizations, you’ll need to set up your communication preference. Choose either email or fax. You can change your preferences at any time.
- For email, we suggest using an email address that others in your office (who handle authorizations) can access because an email can only go to one email address. When an email goes out about an authorization that has posted to the site, the email will be directed to that preferred email address. Then, you’ll need to log in to get the details about your patient.
- Message center: Your message center is your inbox. There, you’ll be able to track messages WholeHealth Living posts about your authorizations, appeals, requests from WholeHealth Living’s Utilization Management Department, or if additional information is needed to complete your authorization request.
When a message is posted, you get an email. Please make sure your system is set up to receive emails from noreply@tivityhealth.com, so messages don’t go into your spam or junk folders.

If you receive an adverse determination and want to appeal the determination, you will have two options for reconsideration.
- Peer to Peer Requests: To request a discussion of the outcome of a clinical review with the peer reviewer who made the determination, please complete and return the "Request for a Peer to Peer Discussion" section of the UM Department Request Form. You’ll find more details on this process in the Chiropractic Services Authorization Program Guide.
- Appeal Requests: If you disagree with a medical necessity review outcome, you have the right to request an appeal. You’ll find more details on this process in the Chiropractic Services Authorization Program Guide.
To request an appeal for a pre-service or concurrent case:
- Please complete and return the UM Department Request Form. Be sure to fill out the "Provider request for a Reconsideration of a Medical Necessity Determination" section.
To request an appeal for a retrospective case:
- Please complete the UM Department Request Form and return it by fax or by mail using the address in your determination letter. Be sure to fill out the "Provider request for an Appeal of a Medical Necessity Determination" section.
WholeHealth Living’s dedicated support line: 1-866-656-6071
![]() Chiropractic Services Authorization Program Guide
Chiropractic Services Authorization Program Guide
![]() Frequently Asked Questions about the Program
Frequently Asked Questions about the Program
To download the Chiropractic payment policy, log in and click Find a Payment Policy on the right side of your home page. Or, go to Office Resources>Policies & Guidelines>Payment Policies.
We use InterQual® Criteria and medical policies to review the majority of authorization requests for commercial members and the Federal Employee Program (FEP). (FEP has its own medical policies.)
We use InterQual® Criteria and medical policies to review the majority of authorization requests for commercial members and the Federal Employee Program (FEP). (FEP has its own medical policies.)
We also publish our payment policies to help providers understand the way a submitted claim will be processed and paid. To access these policies, log in and go to Office Resources>Policies & Guidelines>Payment Policies.
We also publish our payment policies to help providers understand the way a submitted claim will be processed and paid.
Medicare Advantage members
Medicare Advantage coverage determinations are made using Medicare coverage guidelines: CMS National Coverage Determination (NCD) policies and Local Coverage Determination (LCD) policies. When there is no NCD or LCD, we follow our commercial medical policies for Medicare Advantage members. Refer to medical policy 132, Medicare Advantage Management, for a directory of commercial and Medicare policies.
Delegated services
When an authorization program is administered by a vendor, they may use their own clinical criteria to make a medical necessity determination. For more information about specific delegated services, go to Clinical Resources>Prior Authorization.
Federal Employee Program
For members enrolled in the Federal Employee Program (FEP), be sure to visit fepblue.org. On the Medical Policies and Utilization Management Guidelines page, click the tab, Utilization Management Guidelines for guidelines including:
- Inpatient Skilled Nursing Facility Services
- Outpatient High Technology Diagnostic Imaging
- Non-Emergency Air Ambulance Transport
- Hearing Aids
Skilled Nursing Facility Services (FEP Standard Option)
Policies for FEP members can differ substantially from policies for members of commercial or Medicare Advantage plans. Skillled Nursing Facility services for FEP Standard Option members are one example. Refer to the resources below for help following our guidelines.
Dental services covered under the member’s dental benefits
We typically recommend that dentists contact us before performing any services in excess of $250 to determine whether the member has met his/her annual maximum for dental services.
To do this, you may contact the Dental Provider Services at 1-800-882-1178.
Dental services covered under the member’s medical benefits
Some members have coverage for the dental services listed below under their medical benefits. Please note the requirements indicated. In some cases, we will also perform a retrospective review of these services to determine medical necessity.
Temporomandibular Joint Dysfunction (TMJ)
View our TMJ medical policy for authorization and coding information.
Oral surgery rendered in the office
Covered oral surgery services require a referral from a specialist for members of these plans:
- HMO Blue
- Access Blue
- Medicare HMO Blue
We do not require authorization. In some instances, we may contact you to perform a retrospective review of oral surgery services that you perform.
Note: We no longer cover the following services under the member’s medical benefit unless the account has customized the benefit:
- Removal of fully or partially impacted teeth
- Removal of multiple erupted teeth
To check for eligibility and benefits, please call the Dental Provider Service team at 1-800-882-1178, option 3.
Oral surgery rendered as part of an inpatient hospital stay
Authorization is required.
Cleft Lip/cleft palate services
Prior authorization is required for any surgical services related to cleft lip/cleft palate. Prior authorization will not be required for coverage of non-surgical services, but post payment review may occur to ensure that submitted services meet coverage guidelines.
Coverage for these services will be available only if:
- The services are prescribed by the treating physician or surgeon
- The physician or surgeon certifies that such services are medically necessary and consequent to the treatment of the cleft palate, cleft lip, or both
- The orthodontist participates with us and has received prior authorization.
Medically necessary orthodontia
Members under age 19 who have a severe and handicapping malocclusion may qualify for orthodontic care under the Essential Health Benefit mandate if the member belongs to a plan that includes these benefits. Use code D8660 (pre-orthodontic records) to submit claims for the services included in the orthodontic records. You must have an approved prior authorization before beginning treatment; failure to do so will result in a denial of payment. Orthodontic services performed under the Medically Necessary Essential Health Benefit must be completed by an orthodontist specialist.
To request prior authorization, the orthodontist must submit an ADA Dental Claim form, put an X in the box for pre-determinations/pre-authorizations, and include the following documentation:
For comprehensive cases:
- Prior Authorization Request for Medically Necessary Orthodontia Services for Pediatric Essential Health Benefits Form
- Handicapping Labio-Lingual Deviations (HLD Index 4) Form
- Photographic prints (facial, lateral, occlusal)
- Copies of the panoramic and cephalometric radiographic images.
For interceptive cases:
- Photographic prints (facial, lateral, occlusal)
Resources
Blue Book provider manual()Depending on the member’s plan, we may require prior authorization or prior approval for genetic testing.
| For these members | Authorization (or prior approval) is required | Who to contact for prior authorization (or prior approval) |
|---|---|---|
| Commercial HMO/POS members who have a Massachusetts PCP (including New England Health Plan members) |
Yes (for most tests – see below) | Carelon Medical Benefits Management |
| Commercial PPO/EPO plan members | Yes (for most tests – see below) | Carelon Medical Benefits Management |
| Federal Employee Program members | Yes (some tests) | Blue Cross Blue Shield of Massachusetts Clinical Intake department at 1-800-689-7219 |
| Medicare Advantage | Please see the appropriate National Coverage Determination (NCD) or Local Coverage Determination (LCD) through the CMS website for specific genetic testing guidelines | |
Prior authorization program with Carelon Medical Benefits Management (formerly AIM Specialty Health)
For members requiring prior authorization with Carelon (see the table above), here’s some information about the program.
As always, we recommend checking benefits and eligibility to determine the member’s benefits and any authorization requirements before performing services.
Refer to Carelon Genetic Testing Management Program CPT and HCPCS Codes medical policy 957.
Categories of tests that require prior authorization include, but may not be limited to:
- Genetic testing for hereditary risk of cardiac disease
- Genetic testing for hereditary cancer susceptibility
- Genetic testing for single-gene and multifactorial conditions
- Pharmacogenetic and thrombophilia genetic testing
- Reproductive carrier screening and prenatal diagnosis
- Solid and hematologic tumor and malignancy testing
- Whole exome and genome sequencing
Prior authorization is not required for genetic testing associated with organ transplantation.
For preimplantation genetic testing, we don’t require prior authorization with Carelon; however, you should continue to request prior authorization from Blue Cross Blue Shield of Massachusetts for biopsy of the embryo. Refer to our medical policy, Preimplantation Genetic Testing: 088.
Ordering physicians or clinicians must request authorization before the member receives the test (or before performing services). There are three ways to contact Carelon to request prior authorization:
- Through a direct link on this site (no additional registration is required). In the eTools tab, go to Carelon. Click the Go Now button.
- Go directly to the Carelon ProviderPortal (registration is required)
- Go to www.providerportal.com
- Call Carelon’s Contact Center at 1-866-745-1783
- Available Monday through Friday, 8 a.m. – 6 p.m. If you leave a voicemail after these hours, Carelon will respond the next business day.
Here’s some general information you may need to request the authorization. You can find checklists for specific tests on the Carelon genetic testing program site.
- Member’s first and last name, date of birth
- Summary of the patient’s clinical diagnosis
- Ordering provider’s first and last name
- Clinical summary from the genetic counseling appointment
- Test being requested and the name of the laboratory performing the test (you’ll be able to choose the test from a menu that includes branded panels, or you can manually enter it)
- Pedigree or summary of three-generation maternal and paternal family history
- Maternal and paternal ethnic background/race
Tips for entering the date of service for the test
The date of service is the estimated date that the laboratory is likely to begin the testing process.
It is not the date the sample is collected, unless the test is being performed on the same date the sample was collected.
The ordering provider may not know the exact date that a test will be performed. A reasonable estimate of one to three days in the future will cover the vast majority of genetic testing performed.
Once the ordering physician, clinician, or their office staff has entered the required information into the online authorization tool, you’ll get an immediate decision (in most cases). If Carelon needs more time to review the information, the system will indicate that it’s pending review. And, if Carelon needs more information for their review, you’ll get a request to submit additional information.
Please note: When you request prior authorization, it's for a specific genetic test. You aren't requesting prior authorization for the CPT code(s).
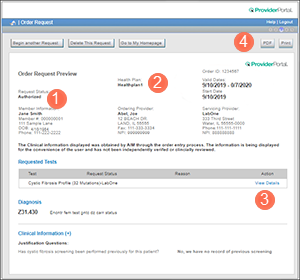
When your authorization is approved, Carelon ProviderPortal will indicate it’s "Authorized" in the Order Request Preview (see ![]() in the example below) You’ll also find:
in the example below) You’ll also find:
- The name of the approved test & CPT code(s)
- The units approved
Please be sure to:
- Tell the member that they must have the test within the timeframe approved (see
 in example). Otherwise, if the test is outside of those dates, a new authorization request will be needed.
in example). Otherwise, if the test is outside of those dates, a new authorization request will be needed. - Attach a copy of the approved authorization to your lab requisition form. This will help the lab understand what's been approved. You’ll be able to download a PDF or print a copy (see
 in example) after you have submitted your authorization request and it’s been approved.
in example) after you have submitted your authorization request and it’s been approved.
- Click "View Details" (
 in example) to see all CPT codes associated with the test that are approved. Remember: You will need to make sure you have approval for each CPT code.
in example) to see all CPT codes associated with the test that are approved. Remember: You will need to make sure you have approval for each CPT code.
- Click "View Details" (
Important: We recommend attaching a copy of the approved authorization to your lab requisition instead of using a pre-populated lab requisition form, such as the one in the example below. When you enter the test into Carelon’s ProviderPortal, you are requesting the individual test, not a panel, so the test authorized and the pre-populated form are not always a match.

Please note: When you request prior authorization, it's for a specific genetic test. You aren't requesting prior authorization for the CPT code(s).
When a specimen comes into your lab for genetic testing, before you analyze the specimen, please remember to verify:
- An approved authorization for the test. You can verify the authorization approval by going to the Carelon ProviderPortal.
- The CPT codes approved as part of that authorization. Next, you can give those codes to your billing department for your claim, so your claims will process smoothly.
- Click "View Details" (See
 in the example above) to see any CPT codes associated with the test that are approved.
in the example above) to see any CPT codes associated with the test that are approved.
- Click "View Details" (See
We’re matching the approved CPT codes and unit amounts to the claim that the laboratory submits. If these fields don’t match, the claim will deny. To avoid a denied claim, we urge clinical and hospital laboratories to use the Carelon ProviderPortal to verify that an authorization is in place before the test is performed. We suggest sharing the authorization approval information (CPT codes and units) with your billing department.
We use Carelon clinical criteria to make medical necessity determinations. Refer to our medical policy 954 for links to Carelon’s criteria.
Blue Cross continues to maintain medical policies for the following:
- Expanded Molecular Panel Testing of Cancers to Identify Targeted Therapies: 790, for which we will continue to maintain the criteria and Carelon will administer prior authorization decisions.
- Preimplantation Genetic Testing: 088, for which the biopsy of the embryo will continue to require prior authorization directly from Blue Cross Blue Shield of Massachusetts, but the associated genetic testing does not require prior authorization if performed for preimplantation genetic diagnosis (as opposed to screening).
- Circulating Tumor DNA and Circulating Tumor Cells for Cancer Management (Liquid Biopsy): 797. We maintain the criteria, but prior authorization should be requested through Carelon.
Carelon offers information on its resource website. You’ll find:
- Program information & clinical guidelines
- Tutorials (on how to enter an authorization using the Carelon online tool)
- Worksheets to help your office prepare the information needed to enter the authorization request
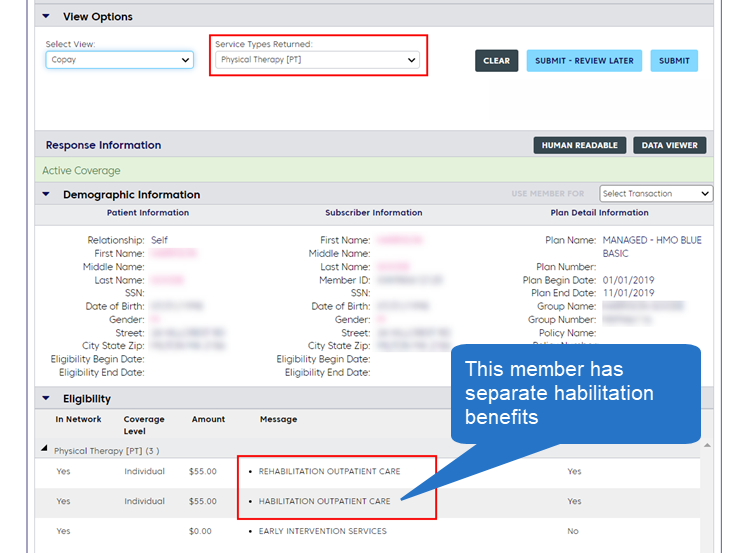
Habilitation services are health care services that help a person keep, learn, or improve skills and functioning for daily living.
Some members have outpatient benefits for habilitation care that are separate from their benefits for rehabilitation care.
For HMO members, authorization is required for these services.
To determine if a member has separate habilitation benefits, perform an eligibility inquiry in ConnectCenterConnectCenter using the Service Type, "Physical Therapy" or "Occupational Therapy." When the member has separate benefits, the Message column in your results will list Rehabilitation and Habilitation separately as shown in the screenshot below.
To request an initial authorization for habilitation services, the PCP or authorized specialist should call Clinical Intake at 1‑800-327-6716. We'll work with you to get an authorization for up to 26 PT/OT (combined) visits in the current calendar year.
To request an extension of an existing authorization, the PCP or authorized specialist should fax us a completed Habilitative Therapy Request Form for HMO Members.
| If the member's benefits are | The PCP or authorized specialist can |
|---|---|
| Combined | Call Clinical Intake at 1-800-327-6716 to request an evaluation visit. Then, if additional visits are needed, we’ll need supporting documentation. Please follow the process for obtaining an outpatient rehab authorization extension for physical therapy or occupational therapy. |
| Separate | Use Authorization Manager to enter an authorization for an initial 26 PT/OT (combined) visits. The authorization period is the current calendar year. |
| If the member's benefits are | The PCP or authorized specialist can |
|---|---|
| Combined | Call Clinical Intake at 1-800-327-6716 to request an evaluation visit. Then, if additional visits are needed, we’ll need supporting documentation. Please fax us a completed Habilitative Therapy Request Form for HMO Members. |
| Separate | Call 1-800-327-6716 to request an authorization for an initial 26 PT/OT (combined) visits. The authorization period is the current calendar year. |
We take a holistic, population-based approach to facilitating appropriate, high-quality, cost-effective care for our members.
Care management programs we offer help address members who are:
- Seriously ill or have complex conditions
- Managing a chronic condition
- At risk for developing serious or chronic illnesses
- Recently hospitalized and could benefit from after care or transitions in care support
We welcome referrals for these programs from physicians, clinicians, members, and their caregivers.
We also offer members additional programs and care support with Other Care Solutions. These offerings help supplement care our members may already be receiving from their health care providers.
To expand access to care for our members, we have complemented our existing network of mental health clinicians by adding mental health groups that offer therapy, medication management, and specialty care to address specific conditions. Many of these mental health groups have:
- In-person and telehealth appointments
- A central intake system for matching and scheduling appointments
- A robust directory of varied provider types
Here’s how to help your patients find care
Need help directing your patients to the right mental health care quickly and efficiently? We encourage you to point them to our MyBlue Mental Health Options page. It’s a tool that streamlines the process of finding a mental health provider for your patients.
Please share this fact sheet and the below simple steps with your patient:
|
|
Sign into your MyBlue account and click on My Care>Mental Health Options. |
|
|
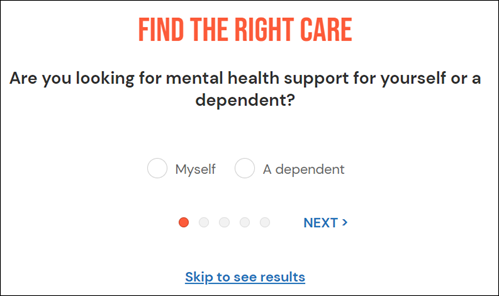
Optional: Answer a brief set of 4-5 questions to assess your specific mental health needs. It can be retaken if needed. |
|
|
Scroll down to see a list of recommended providers. A separate Results for You category will appear only you if answered the optional 4-5 questions mentioned above. |
|
|
Click on Get Started with any of the groups that you think will be a good fit for your mental health needs. You’ll be brought to their websites where you can learn more and easily schedule an appointment. |
Mental health groups
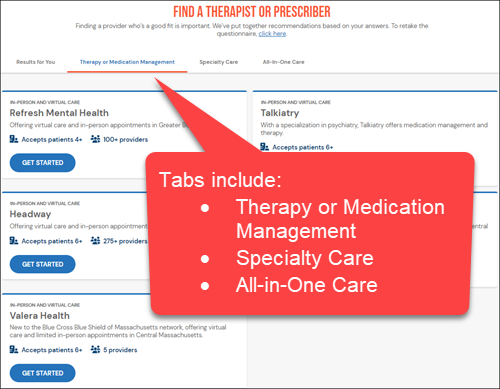
Below is a list of the mental health provider groups your patients will see as options on our site. Click each category to learn more.
If your patient could benefit from a collaborative approach, combining mental health and primary care, then Firefly Health and Carbon Health might be the solution. Both are national provider groups that offer virtual primary and mental health care to our members. Eligible members* can choose a virtual primary care provider associated with either group and get support from a virtual care team to manage their health. Both Firefly and Carbon work closely with mental health providers to give members a collaborative care experience.
*Firefly Health and Carbon Health are currently available to our members with commercial plans (HMO, PPO, and POS). These options will be available to Medicare Advantage and Federal Employee Plan members in the future.
The following groups offer mental health care in-person and virtually, as described below. The clinicians are generalists who provide therapy and medication management. They have an easy-to-use central intake service where members can log on and schedule appointments. These groups strive to schedule our members for their first appointment in a two- to three-day timeframe from the initial call.
| Name | Patient ages accepted | Virtual options offered? | In-person visits offered? |
|---|---|---|---|
| Alma | 5 years and up | Yes | Dependent on each individual clinician |
| Headway | 6 years and up | Yes | Yes |
| Refresh Mental Health | 4 years and up | Yes | Yes |
| Talkiatry | 6 years and up | Yes | No |
| Thriveworks |
6 years and up for therapy
14 years and up for medication management |
Yes | Yes |
| Valera Health | 6 years and up | Yes | Yes |
The following groups offer innovative clinical care among a variety of specialized mental health conditions. Often, these subspecialty groups provide alternatives to residential treatment.
| Name | Areas of focus | Patient ages accepted | Virtual options offered? | In-person visits offered? |
|---|---|---|---|---|
| And Still We Rise | Culturally diverse providers that offer therapy to individuals in diverse communities, including BIPoC (Black, Indigenous, people of color) and LGBTQIA+ individuals | 4 years and up | Yes | Yes |
| Aware | In-home mental health and substance use disorder treatment, including innovative home addiction treatment programs | 18 years and up | No | Yes (in-home) |
| Brightline | On-demand resources and therapy for kids and teens, including a digital platform where families can set up virtual visits and find personalized resources and guides | 3 to 17 years | Yes | No |
| Cortica | Value-based medical care, ABA therapy, counseling, and more for autistic and other neurodivergent children and their families | Birth to 21 years | Yes | Yes |
| DynamiCare | Virtual coaching and treatment of drug, alcohol, and tobacco use, offers financial rewards to encourage healthy behaviors | 13 years and up | Yes | No |
| Eleanor Health | Personalized care plans to help treat substance use disorders and other mental health conditions | 18 years and up | Yes | Yes |
| Forge | Mental health and substance use disorders for active-duty service members, veterans, first responders, and their families | 18 years and up | Yes | Yes |
| NOCD | Virtual care for obsessive compulsive disorder (OCD) through exposure and response prevention (ERP) therapy | 5 years and up | Yes | No |
| Sayftee | Family, individual, couple/relationship, and group therapy and workshops for LGBTQIA+ individuals and the people that love them | 6 years and up | Yes | Yes |
Many of our members have access to Learn to Live, a self-guided, 24/7 online support program based on Cognitive Behavioral Therapy (CBT). The program is intended to help manage social anxiety, depression, stress, anxiety, panic, insomnia, and moderate substance use. It is available in English and Spanish to members 13 and up on fully insured and self-insured accounts that offer this program.
Provider directory
Provider participation: If you need to verify if a particular provider is in our network, you can view our Find a Doctor & Estimate Costs tool.
Keep your directory information up to date: We use the information you enter in CAQH ProView to update our provider directory, so it is important to validate your information quarterly. If you do not keep your data current, or if you do not regularly review and attest to its accuracy, you could be removed from our directory. If you are a facility or group practice, we’ll reach out to you throughout the year to review and validate your information.
For high technology radiology (HTR) services provided in the elective, outpatient setting, we require prior authorization for most commercial HMO/POS, PPO, and Medicare Advantage HMO and PPO. Carelon Medical Benefits Management (formerly AIM Specialty Health) administers this program on our behalf.
Requirements do not apply to Federal Employee Program members. In addition, prior authorization is not required for any member for HTR studies performed:
- In the emergency department
- As part of observation
- In an inpatient setting
- As part of an outpatient surgery
Copayments may apply
For some plans, a member may be responsible for a copayment for certain outpatient radiology studies. As always, check eligibility and benefits before rendering service to determine the member’s cost-share for HTR services.
Ordering clinicians should use eligibility and benefit technologies like ConnectCenter—available 24 hours a day, 7 days a week—to determine what’s required for each of their patients.
Perform your inquiry using the Service Type, MRI/CAT Scan.
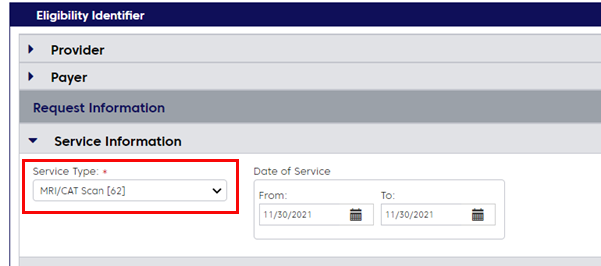
Below is an example of ConnectCenter eligibility search results.
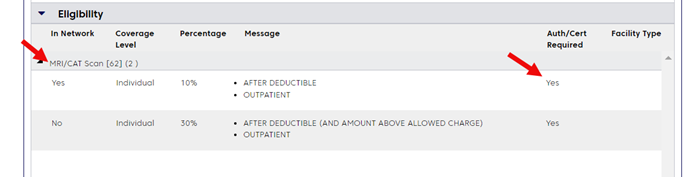
For these services, we require prior authorization for all commercial and Medicare Advantage members:
- Computed Tomagraphy (CT/CTA)
- Magnetic Resonance Imaging (MRI/MRA)
- Nuclear Cardiology Studies
- Breast MRI
- fMRI
- MRS
- Coronary CT/CTA
- CT/PET Fusion
- PET Scans
- Diagnostic and screening colonography
Ordering physicians or clinicians must request authorization before the member receives the test (or before performing services). There are three ways to contact Carelon to request prior authorization:
- Through a direct link on this site (no additional registration is required). In the eTools tab, go to Carelon. Click the Go Now button.
- Go directly to the Carelon ProviderPortal (registration is required)
- Go to www.providerportal.com
- Call Carelon’s Contact Center at 1-866-745-1783
- Available Monday through Friday, 8 a.m. – 6 p.m. If you leave a voicemail after these hours, Carelon will respond the next business day.
Registration is required for web access. When a new provider joins your group, please make sure that clinician is registered with Carelon.
If you are the contracted provider or facility performing the study:
- Register for Carelon as a servicing provider
- Use Carelon’s website to verify whether a prior authorization number has been issued for the member before rendering the service.
Prior authorization is valid for 60 days from the date issued. If the member does not receive the approved test within 60 days, the ordering provider will need to submit a new request.
You will need the following information to make your request:
- Member’s name, ID number, and date of birth
- Ordering provider’s name and address
- Name of imaging facility where the exam will be performed and the date of service
- Type of service (CPT code optional).
- Reason (indication) for the imaging procedure and/or CPT diagnosis code
- Medical records of pertinent previous studies (labs, X-rays, etc.) and treatments, including their duration. This information is critical to the decision-making. If not included, your request is likely to be denied.
- Member’s symptoms
If you are requesting multiple services, please attach medical necessity notes for each service requested.
Carelon will issue a prior authorization number, or forward the case to a nurse or physician for review. The physician reviewer may contact the ordering provider to discuss the case. Ordering providers may also contact Carelon’s physician reviewer at any time during the process.
Carelon is delegated to conduct individual consideration for certain HTR modalities. Here’s more information about the appeals process for HTR services:
| To: | Submit your appeal to: |
|---|---|
|
Carelon Medical Benefits Management c/o Appeals Department 540 Lake Cook Road Deerfield, IL 60015 Fax: 1-800-798-2068 |
|
Blue Cross Blue Shield of MA Provider Appeals P.O. Box 986065 Boston, MA 02298 |
| Plan type | Authorization guidelines |
|---|---|
| HMO/POS EPO, PPO (commercial plans) |
Authorization is not required for services from an in-network home health care provider.
If an HMO or EPO member is receiving care from an out-of-network provider, they will need an approved authorization for coverage because they do not have out-of-network benefits. |
| Medicare HMO Blue | Primary care providers (PCPs) or PCP-referred specialists with an open referral from the PCP may submit a global authorization for home health care services for up to 40 dates of service within 60 consecutive calendar days. These services must be entered as an authorization via electronic technologies.
No review is necessary for Medicare PPO Blue. |
| Federal Employee Program | No precertification is required for Federal Employee program members. For FEP-specific benefit information, call 1-800-451-8124. |
Tips for entering the global authorization (for Medicare HMO Blue members only)
- For Direct ANSI 278 connection, enter the Type of Service code 42.
- For Authorization Manager, follow the instructions in our Quick Tip and User Guide.
- For ConnectCenter, select “Home Health Care” from the Service Type drop-down menu.
Coverage criteria
To qualify for coverage, commercial members must meet InterQual® Home Care guidelines. We use Medicare guidelines to determine coverage for our Medicare Advantage members.
Cases in which the Medicare HMO Blue member requires more than 40 service days are often complex and may be referred to Case Management. Therefore, our Health Management department will review all requests for services beyond 60 dates of service. These services must be entered as an authorization.
If you cannot enter the global authorization because the member has already used the auto-approved home health care services within the time period specified, you will need to contact Health & Medical Management at 1-800-327-6716.
How to request additional services (for Medicare HMO Blue members only)
| If | The home health care provider should fax us these items for case management review | By this time |
|---|---|---|
| Additional home health care services are required beyond the initial auto-approval | A completed Home Health Authorization Extension Request Form and the:
|
At least seven calendar days before the visit limit has expired |
Our nurses will contact the member’s primary care provider, ordering specialist, or home health care agency to review the treatment plan and initiate the extension review process.
When we receive a request for authorization or prior approval, our utilization review nurses use Change Healthcare’s InterQual® criteria to determine if the services and level of care are clinically indicated. If the criteria are met, the case is approved; if the criteria are not met, the case is reviewed by a physician.
InterQual criteria are clinically based on best practice, clinical data and medical literature. They are updated continually and released annually.
Log in to use the Transparency Tool
Blue Cross Blue Shield of Massachusetts makes the criteria available to you through the Transparency Tool. Referring to the criteria in the tool may help you:
| Before a service is rendered: | Determine if it will meet InterQual® criteria. |
| After a service is rendered: | Understand how we made a medical necessity determination for a service that has been rendered. |
To access the InterQual application on our website, log in and go to Clinical Resources>Coverage Criteria & Guidelines>
InterQual Criteria and SmartSheets. Then click Go Now.
Use Authorization Manager
Through our Authorization Manager eTool, Blue Cross Blue Shield of Massachusetts-participating providers can submit initial prior authorization requests for certain back, joint and pain management procedures.
If the CPT code entered requires authorization, the user can go through the medical necessity review process using InterQual subsets (formerly called SmartSheets). If criteria are met and the member’s eligibility is active, the authorization will be approved automatically. If not, the authorization will "pend" for your review and you’ll be notified.
We strive to offer our members the latest in proven medical technologies by reviewing current scientific evidence and considering expert physician opinion when we develop our medical policies. Each month, our Medical Policy Group meets to review the policies for a specific specialty. We incorporate input from the Massachusetts Medical Society, specialty societies, national technology review organizations and community physicians in the development and review of all policies.
Additional information about our medical policies
- Searching for a medical policy? For the best results, search on the medical policy site by category, policy number, procedure code, or alphabetically.
- Medical policies for Federal Employee Program members: Find them on fepblue.org.
- Medical policies for Medicare Advantage members: We are required to make coverage determinations for services through the CMS National Coverage Determination (NCD) policies and benefit manuals. In addition, we follow Local Coverage Determination (LCD) policies established by the Massachusetts Medicare Administrative Contractors. When there is no NCD or LCD, we follow our commercial medical policies for Medicare Advantage members. Refer to medical policy 132, Medicare Advantage Management, for a directory of commercial and Medicare policies.
Providing our members with timely access to mental health care services is a top priority at Blue Cross. Our network of providers offers both in-person and virtual care options to simplify access. Learn more by clicking the links below.
Authorizations & Medical Necessity
Join today!
If you’re not already part of our expansive network of multidisciplinary mental health clinicians, consider joining today. By becoming a Blue Cross Blue Shield of Massachusetts contracted provider, you’ll be part of the solution in helping our members receive personalized and comprehensive support.
Submit a contracting application or learn how to change your status.
Occupational therapy (OT) and physical therapy (PT) services are typically a combined benefit under a member's short-term rehabilitation therapy benefits. Authorization is required for members in the following plans:
- HMO
- POS
- Medicare HMO Blue
- All occupational therapists employed by a group practice must contract with us.
- Authorizations to a occupational therapy group cover only contracted providers. Non-contracted occupational therapists can’t render services to a member, even if an authorization is granted to the group provider NPI.
Reminder: Benefits and benefit limits may vary by account. As always, please check the member’s benefits and eligibility before rendering services.
| For these members | You can request | Within this time period |
|---|---|---|
| Commercial HMO/POS plans | Up to 26 PT and up to 26 OT visits per provider | Per calendar year. |
| Medicare HMO Blue | Up to 12 visits each for PT and OT | Per 365-day authorization period. |
When a patient needs occupational or physical therapy, the member’s primary care provider (PCP) or an authorized specialist is responsible for requesting initial authorization for combined PT/OT visits. (Note: For Medicare Advantage members, only the PCP may submit outpatient rehabilitation therapy authorization requests.)
To do this, the PCP or specialist will need to use a technology. Be sure that you enter the appropriate group PT/OT NPI number. If the member’s maximum visits have already been met for the authorization period, a message will be displayed.
When the request is made electronically, we will automatically approve the initial visits. All authorizations processed in the current authorization period will have the same end date as the initial authorization.
Technologies you can use to submit your request
No authorization is required for members of the Federal Employee Program. However, benefit limits apply for Physical Therapy, Occupational Therapy and Speech Therapy combined.
| If | Then |
|---|---|
| The therapist determines that care beyond the initial visits is needed |
Important:
|
| The member has a new episode of care with the same provider within the same authorization period and the first visits have been used | A new initial evaluation is needed.
The authorization decision will be based on medical necessity criteria. |
To learn the status of an authorization, you can:
- Use an electronic technology like Authorization Manager.
- Enroll in our Automated Fax-back Program to receive daily notices of all service approvals and denials entered into our medical management authorization system for your facility/practice. Enrolled providers receive a Daily Inpatient and Outpatient Notification Report via fax.
For all members except Medicare HMO Blue:
To make medical necessity decisions for initial authorization and extension requests, we use InterQual® Criteria and our medical policies, as described in the subscriber certificate. Visit our InterQual Criteria() page for information about how to access these criteria.
For Medicare HMO Blue members:
We use Centers for Medicare & Medicaid Services (CMS) criteria. Please see the Medicare Benefit Policy Manual.
Total Health Solutions Program
The Total Health Solution (THS) program provides education, targeted outreach, and condition-specific services to Enhanced Dental Benefit members who are pregnant, or have diabetes, coronary artery disease, oral cancer, stroke, Sjogren’s syndrome, intellectual and/or developmental disabilities2, or mental health conditions2.
Enhanced Dental Benefits
Enhanced Dental Benefits offer full coverage for certain preventative and periodontal services connected to the total health of individuals with the conditions shown below. These benefits are paid at 100 percent and are not subject to deductibles, coinsurance, or calendar year maximums when performed by a participating or preferred dental provider.
| Condition | One cleaning or periodontal maintenance1 4 per calendar year | Periodontal scaling once per quadrant every 24 months1 | Oral cancer screening twice per calendar year | Fluoride treatment 4 per calendar year |
|---|---|---|---|---|
| Diabetes |
✔ |
✔ |
|
|
| Coronary artery disease |
✔ |
✔ |
|
|
| Intellectual and/or developmental disabilities 2,3 |
✔ |
|
✔ |
✔ |
| Mental health conditions 2,3 |
✔ |
|
✔ |
✔ |
| Pregnancy |
✔ |
✔ |
|
|
| Oral cancer |
✔ |
|
✔ |
✔ |
| Stroke |
✔ |
✔ |
|
|
| Sjogren’s syndrome |
✔ |
|
✔ |
✔ |
1. Available with plans that offer periodontal maintenance; standard waiting periods apply. There must be at least three months between a periodontal maintenance cleaning and any other cleanings.
2. Self-enrollment is required for this condition.
3. Added on renewal on or after October 1, 2023 and for Dental Blue 65 on January 1, 2024.
Please note: Certain dental plans cover preventive dental services and Enhanced Dental Benefits at different frequency intervals. Please verify the member’s benefits and eligibility prior to scheduling services.
Help your patients take advantage of Enhanced Dental Benefits
If you have a patient with one of the conditions above who is not yet enrolled, follow these steps to get them started:
| Dentists: | Primary care providers: |
|---|---|
|
|
Submit your dental claim electronically or by mail in the same manner as all other dental claims.
Resources
- Fact sheet for providers to help them identify patients who may be eligible for Enhanced Dental Benefits.
- Member fact sheet to hand out to your patients describing the enhanced dental benefits available to them and the importance of good oral hygiene.
- Give the Enhanced Dental Benefits Member Self-Enrollment Form or the Dental Blue 65 Enhanced Dental Benefits Enrollment Form to your patient to have his/her doctor certify a diagnosis that may be eligible for the enhanced dental benefits.
- Dental Blue Book provider manual
Certain members may also have access to programs and additional supports in the following areas:
We offer commercial members in fully insured accounts and Medicare Advantage members a program for chronic back and joint pain with Hinge Health.
Hinge’s pain management program helps adults proactively manage joint and muscle pain through a 12-week, coach-led, digital experience that aims to reduce anxiety and depression, improve strength and mobility, and introduce alternatives to surgery. Participants will continue to have access to all components of the Hinge Health Program, including coaching and/or facilitated social interaction and educational content for 12 months following their engagement in the Hinge Health Program.
We’ll identify eligible members based on claims history for qualified diagnosis codes. Members will then be able to enroll via the Hinge website.
Hinge’s program does not replace the physical therapy benefit for our members, and no claims will be submitted.
This program offers exercise therapy, not physical therapy.
Resource
Member website (commercial members): https://www.hingehealth.com/for/bcbsmafi/
Member website (Medicare Advantage members): https://www.hingehealth.com/for/bcbsmamedicare/
Members 18 and older* have access to virtual visits with Vori Health’s care team for back and joint pain. They are listed on our Find a Doctor & Estimate Costs tool as a Physical Medicine provider. A referral is needed for HMO members and the member’s cost for this virtual care provider depends on their plan.
After an initial telehealth visit, Vori’s care team will develop a treatment plan that may include:
- Physical therapy
- A reduction or change in medication
- Nutrition counseling
- Healthy lifestyle coaching
- Appointments with nurse practitioners or physician assistants as needed
*Commercial members, except Federal Employee Program and plans administered by Blue Benefits Administrators.
Resource
Member website: http://Vorihealth.com/bcbsma
We are partnering with Square Knot Health, an independent company focused on patients with advanced chronic kidney disease (Stage 4, 5, and end-stage kidney disease). This program supplements the care that our Medicare Advantage members receive from their existing doctors by educating, assessing, and mentoring them as they consider treatment options, including transplantation.
Resources
- News article: New chronic kidney disease program for Medicare Advantage members
- Blue Cross Member Medicare Options
- Square Knot Health
Through claims data and other analytics, we navigate members to these care solutions that help complement the care they’re already receiving from their health care providers. Members can learn more on our Diabetes page or call us at the Member Service number listed on their ID card.
As always, members can find doctors, specialists, and durable medical equipment providers (for diabetic equipment and supplies) using our Find a Doctor & Estimate Costs tool.
- Livongo is a diabetes management program that helps adults with type 1 or 2 diabetes to take control of their condition and treatment by introducing a connected blood glucose meter, personalized analytics, and access to coaching, including certified diabetes educators.
- Available to self-insured accounts as an option.
- Transform Diabetes Care supports adults with type 1 or type 2 diabetes with glucose and blood pressure monitoring, preventive screenings, medication optimization and adherence, and lifestyle and nutrition management.
- Support is offered through CVS Pharmacy, CVS MinuteClinic, and CVS HealthHUB locations, as well as remote options.
- Available through our pharmacy benefit manager as a standard benefit to self-insured accounts who use our pharmacy benefits.
Resource
 Transform Diabetes Care member fact sheet
Transform Diabetes Care member fact sheet
- Through a mobile app and a clinical support team, Virta Health helps members reverse their type 2 diabetes without surgery and achieve full remission without medication. They offer nutrition therapy, physician-led care, education, and coaching.
- Is available to qualified adult commercial HMO/POS and PPO members (does not apply to Federal Employee Program members). Eligible members need a smartphone to participate.
Resources
- Virta Health member website: virtahealth.com/join/bcbsma.
- Virta Health fact sheet for providers
For access to virtual specialty care for gastrointestinal conditions:
- Oshi Health’s multidisciplinary clinical support team consists of GI-specialized physician assistants or nurse practitioners, dieticians, GI behavioral health specialists, and care coordinators overseen by board-certified gastroenterologists. They serve as an extension of the member’s care team.
- Available to qualified adult commercial HMO/POS (referral required) and commercial EPO/PPO members (does not apply to Federal Employee Program members).
Resources
Oshi Health member website (commercial members)
![]() Oshi Health fact sheet (for providers)
Oshi Health fact sheet (for providers)
Cost Share Assistance with PillarRx
Offers members savings on high-cost specialty medications through drug manufacturer coupon programs. (Self-insured accounts with 100+ subscribers can opt-in to this product; Fully-insured employers can opt-in with 51+ subscribers; it is a core benefit on merged market plans).
Drug Savings Review
The program uses pharmacy claims to help deliver prescription drug savings and medication optimization through proactive provider outreach (Standard benefit for self-insured accounts).
Pharmacy Advisor
Uses pharmacy claims and social determinants of health data to identify members at risk for non-adherence. Pharmacists provide counseling to members on their medications. (Standard benefit for self-insured accounts).
Medical Cost Avoidance
Analyzes pharmacy and medical claims, plus other data to identify gaps in care. Program engages members in individualized interventions to remind them of the importance of preventive screenings, vaccines, and helps prevent hospital readmissions. (Standard benefit for self-insured accounts).
This medication therapy management program is offered as a service to eligible Medicare Advantage members. It’s offered through pharmacy benefit manager CVS Caremark and Outcomes Inc.
This program is offered at no cost to our members, through our partnership with Carelon Behavioral Health. REACH is designed to help patients with mental health difficulties and/or substance use disorder by arranging care with health care providers to ensure patients feel supported when they leave the hospital. Learn more about REACH.
Maven Clinic offers virtual guidance and support to members and their families throughout the maternity journey*, including:
- Pregnancy
- Doula care
- Postpartum and infant care
- Lactation support
- Return-to-work coaching
- Miscarriage and loss
- Partner support
*The maternity journey includes during pregnancy and within the first three months postpartum; members who recently experienced a pregnancy or infant loss, and a partner of someone pregnant, recently postpartum, or who has recently experienced a pregnancy or infant loss.
What services do they offer?
- Coaching and education through telehealth consultations, and using video and instructional support
- 24/7 access on mobile devices
- Same-day appointments
- Online content, virtual classes, community forums
- Culturally diverse and conscious providers who speak multiple languages
Who is
eligible?
Qualified commercial HMO/POS and PPO members (does not apply to Federal Employee Program members). The Maven maternity program is a core offering for fully insured employers with 51 or more employees. Self-insured accounts can pick from the maternity and newborn care program or offer additional programs that Maven offers in these areas: fertility and family building; parenting and pediatrics; and menopause.
Resource
Maven member website: https://www.mavenclinic.com/
Primary care providers (PCPs) and designated specialists with an open referral from the PCP can refer a member for short-term rehabilitation therapies, including:
Physical therapy
Occupational therapy
Speech therapy
Habilitation Services
In most instances, the benefit for Massachusetts managed care group members is 60 visits per member per calendar year. The 60-visit maximum combines benefits for physical therapy (PT) and occupational therapy (OT) services. Speech therapy (ST) benefits are generally not included in the combined PT/OT short-term rehabilitation benefit. However, some self-funded accounts do combine the three therapies into one benefit.*
As always, it’s important for you to verify member benefits and eligibility before performing services.
*The short-term rehabilitation visit limit for Preferred Blue PPO® and Preferred Blue PPO Basic Saver® is 60 visits. The 60-day outpatient rehabilitation benefit limit does not apply to Medicare HMO Blue.
Telehealth
Visit our telehealth page to learn about telehealth-related payment information, covered services, how to bill, and more.Reimbursement for services is contingent upon:
- Eligibility and coverage. Always remember to verify a member’s benefits and eligibility. Accounts may incorporate riders (for example, to include or exclude out-of-network benefits) on any Blue Cross policy.
- Medical policy. Services must be considered medically necessary according to our current medical policies.
- Coding. Your coding must be consistent with our payment policies, claims review systems, and fee schedules.
For in-network providers:
- Payment is based on your fee schedule. To access your fee schedule, log in and click the Get my fee schedule link on the home page under “I need to….”
- You can collect up-front payment only for the member’s liability (copayment, deductible, or co-insurance).
- You may not balance bill the member for the difference between the allowed amount and your submitted charges.
Reminders:
- Payment is based on your fee schedule.
- You can collect up-front payment only for the member’s liability (copayment, deductible, or co-insurance).
- You may not balance bill the member for the difference between the allowed amount and your submitted charges.
Payment policies
Review our mental health related payment policies:
- Incident To Billing for Supervising Providers for Mental Health Services - Professional
- This payment policy details scenarios in which mental health providers may supervise and bill for services rendered by non-credentialed providers in their practice.
- Community Mental Health Centers
- Mental Health and Substance Use
- Telehealth (Telemedicine) - Medical Services
- Telehealth (Telemedicine) - Mental Health
To download our payment policies, log in and click Find a Payment Policy on the right side of your home page. Or, go to Office Resources>Policies & Guidelines>Payment Policies.
Review our mental health related payment policies:
![]() Incident To Billing for Supervising Providers for Mental Health Services - Professional
Incident To Billing for Supervising Providers for Mental Health Services - Professional
- This payment policy details scenarios in which mental health providers may supervise and bill for services rendered by non-credentialed providers in their practice
![]() Community Mental Health Centers
Community Mental Health Centers
![]() Telehealth (Telemedicine) - Medical Services
Telehealth (Telemedicine) - Medical Services
![]() Telehealth (Telemedicine) - Mental Health
Telehealth (Telemedicine) - Mental Health
Psychiatric collaborative care management (CoCM)
See our detailed CoCM fact sheet to learn about this model that integrates mental health care into primary care and how to bill for it.
Billing information for children and adolescents
In accordance with the Massachusetts Division of Insurance (DOI), we cover certain mental health services to address emotional and behavioral conditions found in children and adolescents under age 19. This includes services such as In-Home Therapy (IHT) and Intensive Care Coordination (ICC).
For a comprehensive list of the treatments we cover, how to bill for them, and commonly asked questions, see our Behavioral Health for Children and Adolescents (BHCA) fact sheet.
Child psychiatry incentive program (CPIP)
If you are a child psychiatrist, you can learn about our incentive program by logging into Provider Central and going to Quality & Performance> Performance Programs>Child Psychiatry Incentive Program.
Child psychiatry incentive program (CPIP)
If you are a child psychiatrist, you can learn about this program by visiting our Child Psychiatry Incentive Program page.
Occupational therapy (OT) and physical therapy (PT) services are typically a combined benefit under a member's short-term rehabilitation therapy benefits. Authorization is required for members in the following plans:
- HMO
- POS
- Medicare HMO Blue
- All physical therapists employed by a group practice must contract with us.
- Authorizations to a physical therapy group cover only contracted providers. Non-contracted physical therapists can’t render services to a member, even if an authorization is granted to the group provider NPI.
Reminder: Benefits and benefit limits may vary by account. As always, please check the member’s benefits and eligibility before rendering services.
| For these members | You can request | Within this time period |
|---|---|---|
| Commercial HMO/POS | Up to 26 PT visits and up to 26 OT visits per provider | Per calendar year. |
| Medicare HMO Blue | Up to 12 visits each for PT and OT | Per 365-day authorization period. |
When a patient needs physical or occupational therapy, the member’s primary care provider (PCP) or an authorized specialist is responsible for requesting initial authorization for combined PT/OT visits. (Note: For Medicare Advantage members, only the PCP may submit outpatient rehabilitation therapy authorization requests.)
To do this, the PCP or specialist will need to use a technology. Be sure that you enter the appropriate group PT/OT NPI number. If the member’s maximum visits have already been met for the authorization period, a message will be displayed.
When the request is made electronically, we will automatically approve the initial visits. All authorizations processed in the current authorization period will have the same end date as the initial authorization.
Technologies you can use to submit your request
- Authorization Manager. Follow the instructions in our Quick Tip and User Guide.
- Direct Connection.
No authorization is required for members of the Federal Employee Program. However, benefit limits apply for Physical Therapy, Occupational Therapy and Speech Therapy combined.
| If | Then |
|---|---|
| The therapist determines that care beyond the initial visits is needed |
Important:
|
| The member has a new episode of care with the same provider within the same authorization period and the first visits have been used | A new initial evaluation is needed.
The authorization decision will be based on medical necessity criteria. |
To learn the status of an authorization, you can:
- Use an electronic technology like Authorization Manager.
- Enroll in our Automated Fax-back Program to receive daily notices of all service approvals and denials entered into our medical management authorization system for your facility/practice. Enrolled providers receive a Daily Inpatient and Outpatient Notification Report via fax.
For all members except Medicare HMO Blue:
To make medical necessity decisions for initial authorization and extension requests, we use InterQual® Criteria and our medical policies, as described in the subscriber certificate. Visit our InterQual Criteria() page for information about how to access these criteria.
For Medicare HMO Blue members:
We use Centers for Medicare & Medicaid Services (CMS) criteria. Please see the Medicare Benefit Policy Manual.
We review certain inpatient and outpatient services to determine if they are medically necessary and appropriate for the member. If we determine that the services are medically necessary, we send an approval—or authorization—in writing to the member, primary care provider (PCP), the treating physician, and the facility, if applicable, to let them know that we have approved the services.
When a request for service is not approved, we notify the PCP* and the member.
*When the member has a PCP.
Before performing a service that requires an authorization, you should take these steps:
| Step |
Use an eTool like Authorization Manager or ConnectCenter to determine whether a referral or authorization is required for a specific service. Learn about our eTools.
Once you’ve checked member benefits and eligibility, our Inpatient Only List can help you in making level of care determinations. Please also refer to our medical policies.
|
| Step |
Submit your authorization request (see submission tips below). |
| Step |
Check the status of your authorization request.
|
| Step |
Perform the service and submit the claim (after you’ve confirmed you have an authorization on file for the service). |
Either the primary care provider or the designated specialist (with an open referral from the primary care provider, as applicable depending on the plan) can request authorization for outpatient services. If we have not provided approval for outpatient services that require authorization, the provider rendering the service is financially liable, unless the member has previously consented in writing to be billed.
| For | Please |
|---|---|
| Level of care authorization upon admission, concurrent reviews, and transfers between facilities for premature and medically complex infants in the NICU |
Contact ProgenyHealth:
|
| Inpatient and outpatient medical and behavioral health authorization requests |
|
| 278 transactions | Refer to our Direct Connection page for more information. |
| Federal Employee Program members | Contact Ancillary Services at 1-800-451-8124 for FEP specific benefit |
| Fax or mailed authorization requests | Use Mass Collaborative's Prior Authorization Request Forms
|
| BlueCard Members’ pre-service review (for out-of-area members or members of another Blue Plan) | Use the Pre-service Review for BlueCard Members tool. Or call 1-800-676-BLUE. |
We urge you to check on the status of your authorization requests electronically. If you have questions once you’ve taken this step, you may reach us at the phone and fax numbers indicated below.
Phone information
| For: | Call: |
|---|---|
| Medical pre-authorizations and referrals | 1-800-327-6716 |
| Behavioral health authorizations | 1-800-524-4010 |
Fax information
| For: | Fax: |
|---|---|
|
Medical pre-authorizations and referrals:
|
1-888-282-0780 |
| Emergent Inpatient Notification | 1-866-577-9678 |
|
If we request additional clinical:
|
1-888-282-1321
|
| Outpatient Physical, Occupational and Speech Therapy authorizations | 1-866-577-9901 |
| InterQual Smart Sheets TM Surgical forms | 1-888-641-1375 |
| IVF authorizations and referrals | 1-800-836-1112 |
| Skilled nursing facility, rehabilitation hospital, inpatient hospice and respite | 1-888-641-5330 |
|
Behavioral Health:
|
1-888-641-5199
|
| Federal Employee Program Plans | |
| Federal Employee Plan: Authorizations and InterQual Smart Sheets TM Surgical Forms | 1-888-282-1315 |
| Federal Employee Plan: Additional requested clinical information | 1-866-577-9682 |
| Medicare Plans | |
| Medex®' : Authorizations and referrals | 617-246-4210 |
| Medicare Advantage: Authorizations and referrals | 1-800-447-2994 |
| Medicare Advantage: Additional requested clinical information | 1-866-577-9682 |
| Medicare Advantage: Skilled nursing facility and rehabilitation hospital | 1-800-205-8885 |
| Blue Cross Blue Shield of Massachusetts Employees | |
| BCBSMA employees: authorizations, referrals and InterQual Smart Sheets TM Surgical forms | 617-246-4299 |
| BCBSMA employees: behavioral health/substance use authorizations and neuropsychological testing | 1-888-608-3693 |
Resources for mental health clinicians, primary care providers, and their patients.
Mental Health Brief
Our quarterly Mental Health Brief e-newsletter helps you stay informed about Blue Cross news that affects you. Here are the past issues:
![]() October 2020
October 2020
![]() March 2021
March 2021
![]() July 2021
July 2021
![]() November 2021
November 2021
![]() May 2022
May 2022
![]() November 2022
November 2022
![]() March 2023
March 2023
![]() June 2023
June 2023
![]() September 2023
September 2023
![]() February 2024
February 2024
Webinars
October 25, 2023: Tools and resources for mental health providers
Quick Tips
![]() CBHC Quick Tips: for community mental health centers (CMHCs) providing emergency community behavioral health care (CBHC) services for our members
CBHC Quick Tips: for community mental health centers (CMHCs) providing emergency community behavioral health care (CBHC) services for our members
Coverage
Coverage is our health news service that reports on important health issues, including mental health stories and testimonials.
Treatment resources
See our list of Treatment Resources that span a wide range of mental health conditions, including Attention-deficit/hyperactivity disorder (ADHD), alcohol and substance abuse, depression, and post-partum depression.
Medications and substance use
- Use our medication lookup tool to see which drugs are part of our formulary.
- Visit our opioid resource center for helpful information and resources.
Resources for members
We have a dedicated mental health page on our member website, MyBlue. Share our MyBlue Mental & Behavioral Health page with your patients so they can learn about all of the resources available to them.
Prior authorization requirements for sleep testing and treatment
For these services, we require prior authorization for all commercial and Medicare Advantage members. Authorization is not required for Federal Employees Program (FEP) members.1
|
|
|
|
|
|
How to submit a prior authorization request
Carelon Medical Benefits Management (formerly AIM Specialty Health) is the company that administers the prior authorization program for us. Carelon uses our medical policies to identify the clinical appropriateness of home or lab testing:
- Sleep Disorder Management (969)
- Sleep Disorder Management CPT and HCPCS Codes (970)
- Medicare Advantage High Tech Radiology and Sleep Disorder Management (923)
On our medical policy site, search for "sleep."
Ordering clinicians
Ordering physicians or clinicians must request authorization before the member receives the test (or before performing services). There are three ways to contact Carelon to request prior authorization:
- Through a direct link on this site (no additional registration is required). In the eTools tab, go to Carelon. Click the Go Now button.
- Go directly to the Carelon ProviderPortal (registration is required)
- Go to www.providerportal.com
- Call Carelon’s Contact Center at 1-866-745-1783
- Available Monday through Friday, 8 a.m. – 6 p.m. If you leave a voicemail after these hours, Carelon will respond the next business day.
Free-standing labs, hospitals, and DME vendors
Check with Carelon to make sure an authorization is in place before rendering services. Authorization for ongoing sleep therapy supplies will be dependent on member utilization of the equipment. The DME vendor will be required to provide utilization data to Carelon when requesting authorization for ongoing treatment.
1. For FEP, prior approval is required for sleep studies performed in a location other than the home. Fax prior authorization requests to us at 1-888-282-1315.
Speech therapy services can sometimes be a combined benefit under an HMO/POS member’s short-term rehabilitation therapy benefits. For members of our Medicare HMO Blue Plan only, we require authorization for the initial 30 visits.
- All speech therapists employed by a group practice must contract with us.
- Authorizations to a speech therapy group cover only contracted providers. Non-contracted speech therapists can’t render services to a member, even if an authorization is granted to the group provider NPI.
When a patient needs speech therapy, their primary care provider (PCP) or an authorized specialist is responsible for generating an auto-approved initial authorization for the first 30 visits, every 365 days.
To do this, the PCP or specialist will need to use a technology. If the member’s maximum visits have already been met for the 365-day authorization period, a message will be displayed.
Technologies you can use to submit your request
No authorization is required for members of the Federal Employee Program. However, benefit limits apply for Physical Therapy, Occupational Therapy and Speech Therapy combined.
| If | Then |
|---|---|
| The speech therapist determines that care beyond the initial 30 visits is needed |
|
| The member has a new episode of care within the same 365-day period and the first 30 visits have been used |
The authorization decision will be based on medical necessity criteria. |
To learn the status of an authorization, you can:
- Use an electronic technology like Authorization Manager.
- Enroll in our Automated Fax-back Program to receive daily notices of all service approvals and denials entered into our medical management authorization system for your facility/practice. Enrolled providers receive a Daily Inpatient and Outpatient Notification Report via fax.
We use Centers for Medicare & Medicaid Services (CMS) criteria. Please refer to the Medicare Benefit Policy Manual.
These medical and mental health resources include clinical guidelines and educational information that can help your patients—our members—to manage their care.
Medical
Preventive and primary care
| Resource | Source |
|---|---|
Clinical guidelines:
|
Massachusetts Health Quality Partners (MHQP) |
| Blue Cross Blue Shield of Massachusetts | |
| HPV vaccination fact sheet for dental and medical patients |
|
| Smoking cessation: TryToStop.org or 1-800-QUIT-NOW Smoking cessation programs are available to all members at no cost |
Massachusetts Department of Public Health |
For your convenience, we created preventive care reminder letters your office can use as templates.
Osteoporosis
| Resource | Source |
|---|---|
| STEADI Program STEADI provides training, tools, and resources for health care providers to help prevent falls and help their patients stay healthy, active, and independent longer. |
Centers for Disease Control and Prevention (CDC) |
Pain management/opioids
See also the Alcohol and Substance Use section below.
| Resource | Source |
|---|---|
| AGS Beers Criteria® for Potentially Inappropriate Medication Use in Older Adults | The American Geriatrics Society (AGS) |
| Pocket Guide: Tapering Opioids for Chronic Pain | Centers for Disease Control and Prevention (CDC) |
| Managing Chronic Pain in Adults With or in Recovery From Substance Use Disorders | Substance Abuse and Mental Health Services Administration |
|
View our formularies for coverage information. |
Blue Cross Blue Shield of Massachusetts |
| Our Opioid Resource Center | |
Medical policies including:
|
|
| Pharmacy information |
Mental health
Alcohol and substance use
| Resource | Source |
|---|---|
| Clinical practice guidelines | American Psychiatric Association |
| Medication Assisted Treatment for Opioid Addiction in Opioid Treatment Programs | Substance Abuse and Mental Health Services Administration |
| Systems-Level Implementation of Screening, Brief Intervention, and Referral to Treatment (SBIRT) | |
| Our Opioid Resource Center | Blue Cross Blue Shield of Massachusetts |
Attention deficit hyperactivity disorder (ADHD)
| Resource | Source |
|---|---|
| ADHD Resource Center Includes Practice Parameter for the Assessment and Treatment of Children and Adolescents with Attention-Deficit/Hyperactivity Disorder |
American Academy of Child and Adolescent Psychiatry |
| Attention-Deficit/Hyperactivity Disorder | National Institute of Mental Health (NIMH) |
| Pediatric Symptom Checklist (PSC) The Pediatric Symptom Checklist is a brief screening questionnaire used by pediatricians and other health professionals to recognize psychosocial problems and improve treatment in children. |
Massachusetts General Hospital |
| Blue Cross Blue Shield of Massachusetts |
Depression
| Resource | Source |
|---|---|
| Clinical practice guidelines | American Psychiatric Association |
| Blue Cross Blue Shield of Massachusetts |
Post-partum depression
| Resource | Source |
|---|---|
| Edinburgh Postnatal Depression Scale (EPDS): |
American Academy of Pediatrics |
Educational resources for members
- Bluecrossma.org offers our members resources for everyday wellness and certain conditions, like substance use disorder, asthma, and pregnancy.
- Fepblue.org offers Federal Employee Program members wellness resources and health tools.
Clinical practice guidelines referenced on this site are intended as a guide for treatment and do not represent a standard of care for a member with a specific disorder. The guidelines are not a substitute for individualized assessment and treatment planning, and services recommended under the guidelines will not always be determined to be medically necessary. Claim payment decisions are based on the member's benefits, eligibility, coverage, and benefit limitations at the time the service is being performed.