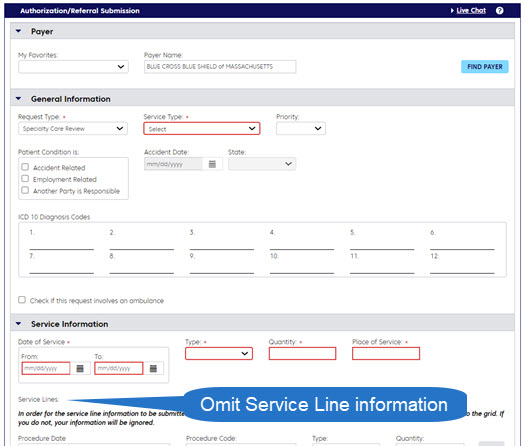
You can manage referrals electronically using Authorization Manager, ConnectCenter, or a Direct Connection. Learn more about our technologies.
Note: A referral does not guarantee reimbursement. Member benefits and medical and payment policies may affect coverage and reimbursement.
Entering referrals
You can use eTools to enter and check referrals for all members in managed care plans, including those out of area. Referrals can be entered for up to 99 visits, and are good for 365 days.
Important note for Authorization Manager: Procedure code 99243 is required, as well as a diagnosis. If no diagnosis is available, you may enter general symptoms (R68.89). Then continue as you would with an authorization request.
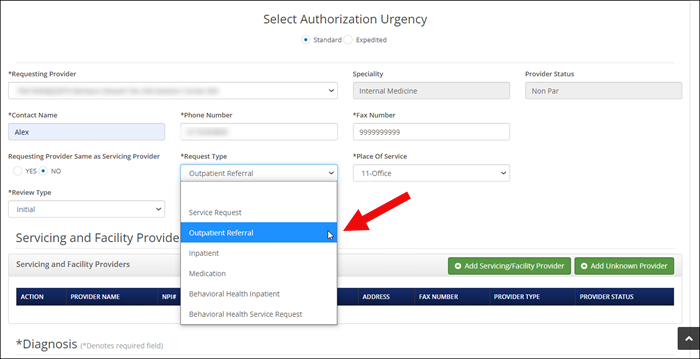
Verify referrals before rendering services
Verifying that a referral is on file and that the number of requested visits matches the services required helps facilitate the claims process and avoids unnecessary appeals or inquiries.
To search for an existing referral in Authorization Manager go to the View Authorizations screen. You can filter your list by typing "referral" under the column heading, Request Type.
With Authorization Manager, you can see both the Requesting Provider and the Servicing Provider.
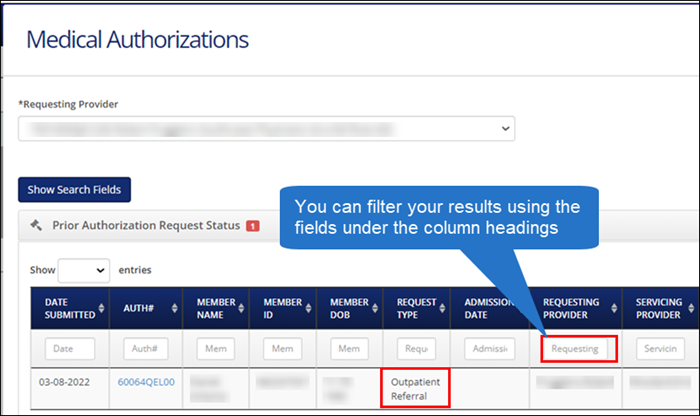
To verify a referral in ConnectCenter, go to Verification> Authorization/Referral Status. Complete the required fields and click Submit.
- For Provider Type, select "Specialist" for any individual provider (non-facility).
If a referral is active, your results will look like this:
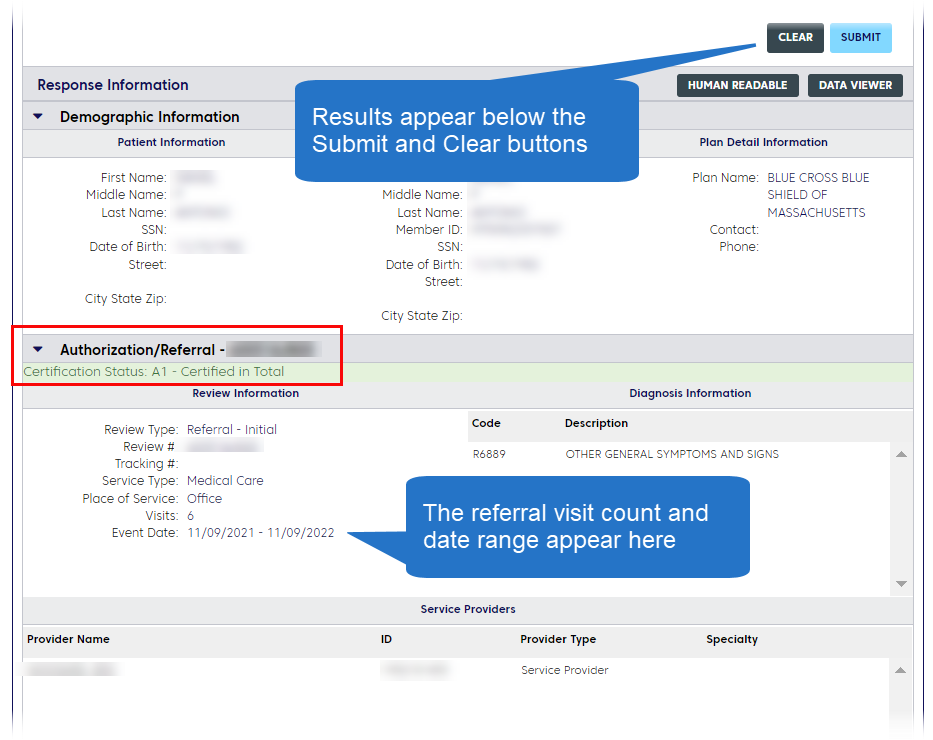
A primary care provider may recommend that a member consult with a specialist for care that the primary care provider can't provide. This is called a referral. The following managed care plans require notification of a referral for specialist care:
- Blue Choice® (in-network HMO providers only)
- HMO Blue
- Network Blue®
- Managed Blue for Seniors
- Medicare HMO Blue
Specialist providers: For NEHP members with out-of-state PCPs, confirm the referral was received by the member’s home plan (which may not be Blue Cross Blue Shield of Massachusetts).
The primary care provider is responsible for coordinating the member’s care and entering the referral before the service is provided (at least one business day). A referral is valid for 365 days and allows the member to see a specialist for a certain number of visits (1-99).
- Please use a technology like ConnectCenter to check whether a referral is in place before treating a managed care member.
- If there is no referral on file, please contact the member’s primary care provider. If you treat a patient without a referral, you cannot bill the member for the service unless you get the member’s prior written consent stating that they will be responsible for payment.
- To ensure that the member understands the written consent allows you to collect fees for non-covered services, the member must sign the waiver on the date of service. It does not need to list the specific service that won’t be covered, but it should indicate that if the member does not have the required referrals, the member will be responsible for charges that are not covered.
- If your initial claim is rejected due to lack of a referral, verify that the primary care provider submitted the referral, and submit a replacement claim within the timely filing limit.
If, for some reason, a referral cannot get entered before the service is performed, it can be submitted retroactively up to 90 days from the date of the actual visit. Enter the actual date of service as the start date.
Behavioral health services, urgent care, and Emergency Department services (for emergency conditions) don't require a referral.
You may need to request an authorization for coverage of some of these services. Either the primary care provider (PCP) or the designated specialist (with an open referral from the PCP, as applicable depending on the plan) can request authorization for outpatient services.
Please use an eTool to check the member's benefits and go to Clinical Resources>Prior Authorization for more information.
In addition, the following outpatient services don't require a referral when provided by an in-network provider:
- Routine hearing exams
- Nutritional counseling
- Routine vision exams. Most HMO members now have coverage for one routine vision exam every 24 months. However, some employers opt to modify these guidelines, so be sure to verify the members’ benefits before rendering care. (Medical eye care visits do not have the 24-month limit.)
- The following specialty-care services provided by a plan obstetrician, gynecologist, certified nurse midwife or family practitioner:
- Annual preventive gynecological exam (including any subsequent medically necessary OB/Gyn services). Please note: Medicare Advantage members require a referral for medically necessary OB/Gyn services.
- Maternity care
- Medically necessary evaluations and resulting health care services for acute or emergency gynecological conditions.
- Certain durable medical equipment, including apnea monitors and oxygen. Specific durable medical equipment items require medical policy review; for example, wound vacs and specialty beds. Please check benefits and eligibility before providing services to determine member’s cost share and durable medical equipment limits, if any.
- Initial home health care visit for early maternity discharges
- Dialysis
- Outpatient hospice services, including home health aide visits, drugs, durable medical equipment, skilled nursing visits, respite care and bereavement services. However, authorization is required for any home infusion therapy services provided as part of hospice care. For Medicare Advantage (Medicare HMO Blue and Medicare PPO Blue) members, hospice services are covered under the member’s Medicare benefit.
- Acupuncture