This article is for:
- Home health care providers
- Mental health clinicians
- Providers who recommend home health care services to our members

We recently announced that we have eliminated authorization requirements for home health care services for our commercial members. This is intended to ease administrative burden and provide quick access to our members who need home care services—especially those being discharged from an inpatient facility who want to continue treatment at home.
Here we answer questions we’ve received from home health care agencies about this announcement and share information about our home health care benefit as it relates to mental health services.
For dates of service on and after January 1, 2024:
- We no longer require a global authorization for our commercial HMO, POS, EPO, and PPO1 members. You also do not need to request authorization throughout the episode of care.
- This applies to home health care services provided by an in-network agency, such as skilled nursing care; physical, occupational and speech therapy; social work; and home health aide services.
- You don’t need to add an authorization number to your claims. Our claims system will process the claim by the date of service. If you need a retroactive authorization for a service before December 31, 2023, please call us at 1-800-327-6716 or fax the request to 1-888-282-0780.
1 Federal Employee Program members already do not require authorization.
We continue to require authorization for:
- Medicare HMO Blue members. Please follow your existing processes for Medicare HMO Blue members.
- Home infusion therapy services for all members.
- Private duty nursing for plans that offer this benefit.
We don’t require referrals for home health care services. Orders can be written by the member's treating provider—PCP, psychiatrist, or other specialty.
Use an online tool, such as ConnectCenter, to check member benefits and eligibility.
If you’d like to see if the member has a benefit maximum for home health care services, see our ConnectCenter Quick Start Guide (screenshot below) for instructions.
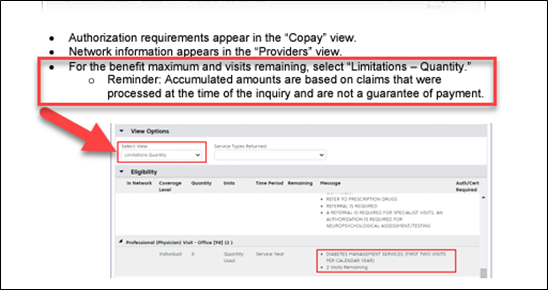
For commercial members, we use InterQual®' criteria to determine medical necessity. To access the InterQual criteria, you’ll need to log on to Provider Central and navigate to Clinical Resources>InterQual Criteria. Click the “Go now” button and select “LOC: Home Care Q & A” to access them.
For commercial members, we use InterQual®' criteria to determine medical necessity.
For Medicare Advantage members, we use CMS’ criteria.
Keep in mind that members with mental health conditions may qualify for home health care services, just as members with physical conditions do. For example, patients may be eligible for home health services if they are recently discharged from an inpatient stay at an acute care hospital or a behavioral health hospital and need medication administration support for injectable medications.
Here's how this might work:
- An HMO member needs psychiatric care.
- If the psychiatrist determines that the patient needs home health care (for example, to help them inject their medication), the psychiatrist’s office would coordinate the care with the home health care organization.
- The home health care agency will need doctor's orders from the psychiatrist.
- No global authorization is required.
Resources
- Home health care page
- InterQual Criteria
- InterQual Criteria (log in required)
- ConnectCenter: For member eligibility and benefits verification, claim status, and more. You’ll find tips, resources, and other information to help support your use of the tool
- Authorization Manager: To check authorization requirements
MPC_091923-2Y-3-ART