ConnectCenter Tips: Provider Management
May 25, 2022
This article is for providers who currently use Online Services for eligibility and benefits queries and claim submission
As you begin to explore ConnectCenter, we want to provide you with some quick knowledge to help you get started. In this article, we’ll focus on Provider Management, which is found under the Admin tab.
The Provider Management area in ConnectCenter allows you to:
- create provider records that you can use throughout the application
- create provider defaults to maximize your efficiency.
Note: If you previously entered claims using Online Services, Change Healthcare has transferred your provider information to ConnectCenter. Please review these records before using them in transactions or claims. It is very important that you do not create duplicate provider records.
How to create provider records in ConnectCenter
- From within ConnectCenter, go to Admin>Provider Management and click
Create.
- The Create/Edit Provider screen appears. You will be prompted to enter an ID number. Enter the provider’s NPI and hit the Tab key on your keyboard. This will check the NPI you provided against the National Plan and Provider Enumeration System (NPPES).
If the NPI is found in the NPPES registry, data from the registry will be populated into ConnectCenter. If the data from the registry is out-of-date, you can and should correct it.
- Enter or correct provider details as needed.
- Look for the section marked “Set Provider As Default.”
- To use the provider as a default provider for real-time transactions (benefits, eligibility, and claim status), click the check box, “Requesting Provider.”
- To use the provider as a default in 1500 claim submissions, check “Billing Provider” or “Rendering/Performing Provider.”
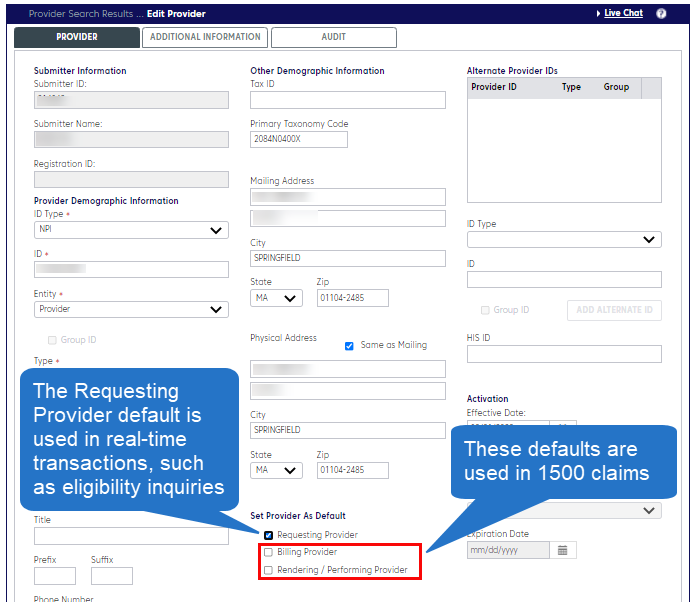
Click Save to use the provider information in your transactions.
MPC_062321-2L-46