Please share this information with your staff who perform eligibility and benefit inquiries for your Blue Cross patients
The following ConnectCenter tips have been created for providers who perform eligibility inquiries to find out specific benefit details, such as:
- the dates of a service year
- the number of visits allowed and remaining.
The Coverage Status area
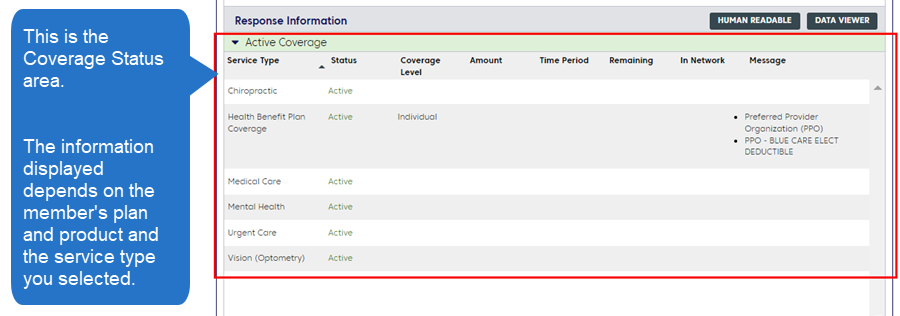
Submit your eligibility inquiry with the most appropriate Service Type. If the member is enrolled in a Blue Cross plan, your results will include the words “Active Coverage” in a green bar. The area under the bar may list categories of coverage. This is the Coverage Status area.
Depending on the member’s plan and product, the Coverage Status area may be detailed or simple.
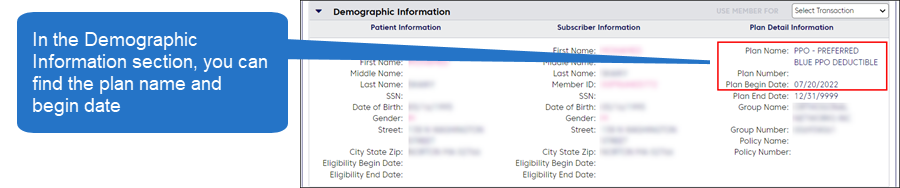
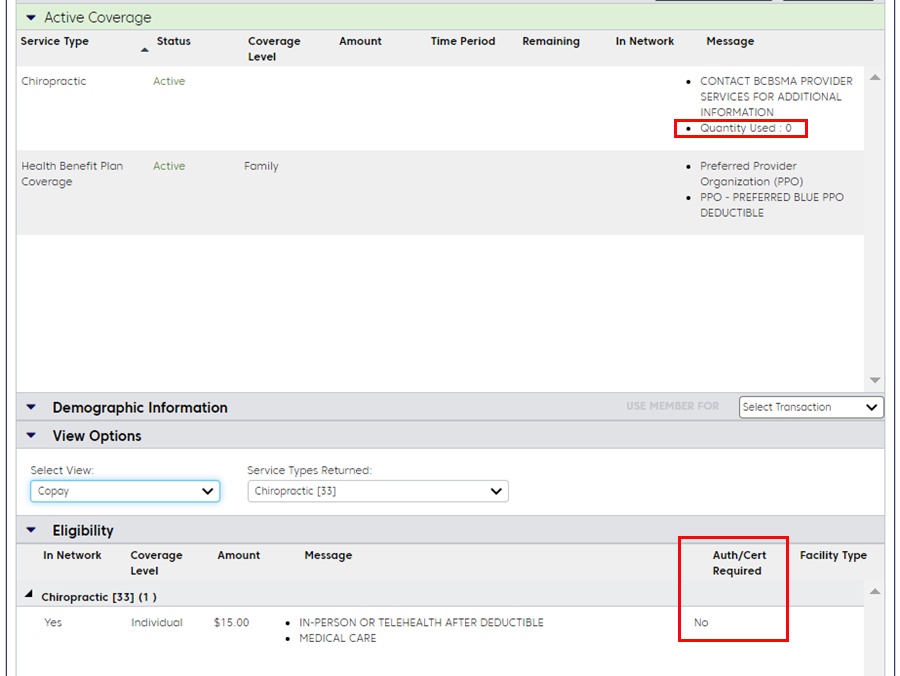
The example below shows the results for an inquiry using the service type, “Chiropractic.” The Coverage Status area shows that this member is in a PPO plan and has not used chiropractic benefits in their service year.
We can also see, in the Eligibility area, that no authorization is required. Because most PPO plans include authorization requirements for visits 13 and beyond, it’s likely that this member has a benefit limit of 12 visits.
View Options
After reviewing the Coverage Status area, scroll to the View Options area. This is where you can change which portion of the plan’s response is displayed under “Eligibility.” For most members, the default view will be Copay.
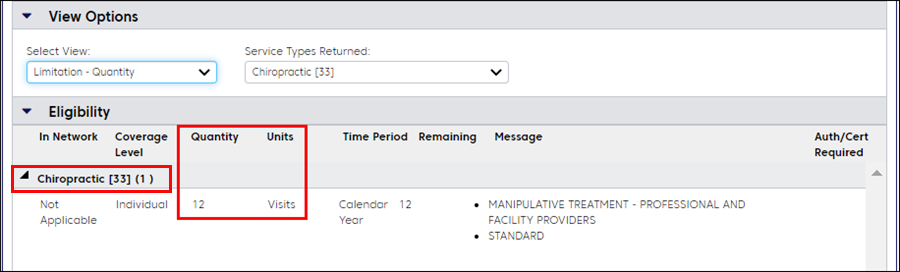
In the example below, for a Medex member, the selected view is Limitation – Quantity.
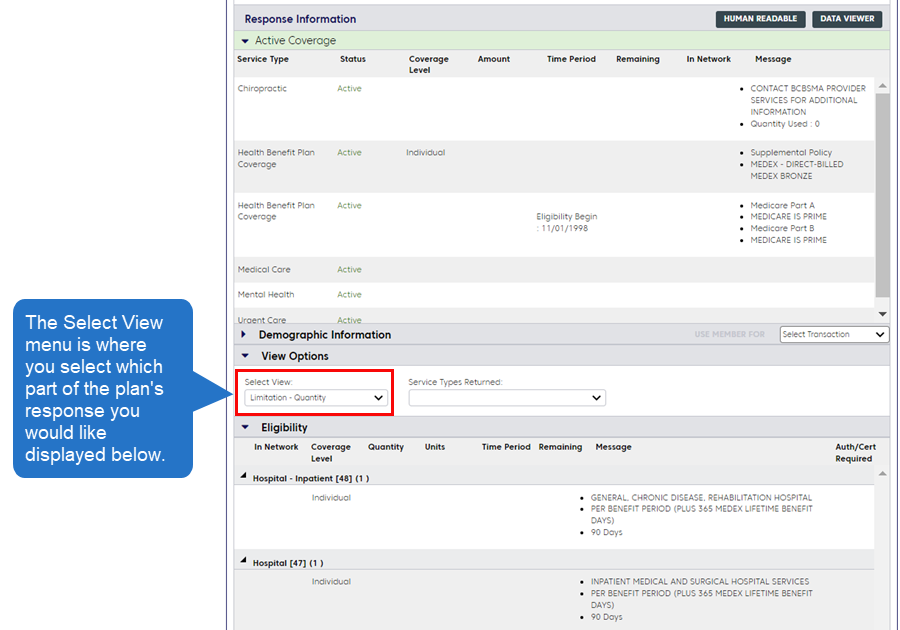
Here is an example for a Federal Employee Program member with coverage for 12 chiropractic visits per calendar year. Twelve visits are remaining.
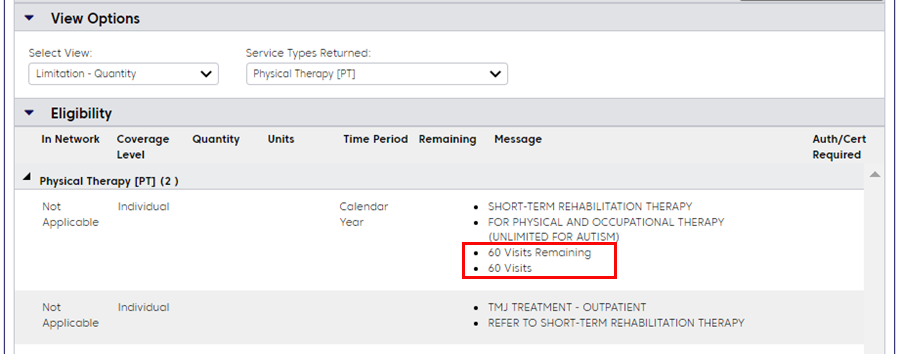
The member below is also in a PPO plan. We can see that they have:
- Combined benefits for physical and occupational therapy
- A benefit limit of 60 visits per calendar year
- 60 visits remaining
MPC_062321-2L-118