Chiropractors should request continued review for chiropractic services for certain Blue Cross Blue Shield of Massachusetts members. WholeHealth Living, Inc., a Tivity Health Company, administers the program.
Many, but not all, members in these plans need continued review for chiropractic services. Please check benefits and eligibility to determine if continued review is required.
| Plan name | Additional information |
|---|---|
| HMO/POS plans | |
| HMO Blue Blue Choice Plan 2 Network Blue |
If the member has a 12 visit limit to their chiropractic benefits, continued review doesn't apply. |
| HMO/POS New England Plans (some account exclusions apply) | |
| Access Blue New England HMO Blue New England Network Blue® New England Blue Choice® New England (POS) Blue Choice® New England Plan 2 (POS) |
Includes members who:
|
Use ConnectCenter to see if the member requires continued review.
Go to Verification>New Eligibility Inquiry and complete required fields. Click Submit.
Scroll to view the response. Under Eligibility, look for Chiropractic. If continued review is required, you'll see a message indicating continued review is required for visits 13 and beyond.
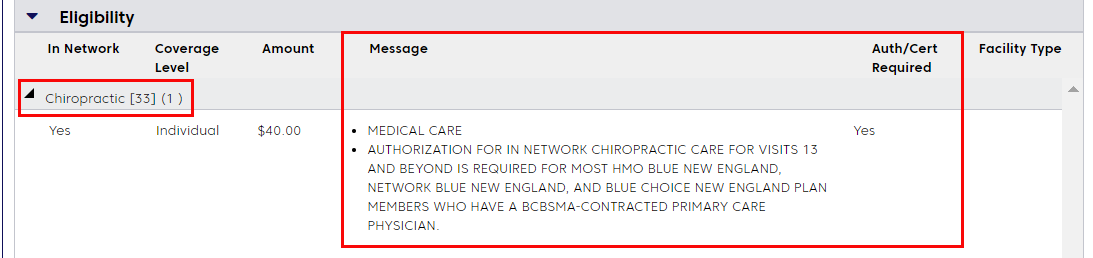
If continued review is not required, you'll see a message like the one below. This message may appear if the member has a 12 visit benefit limit for chiropractic services.
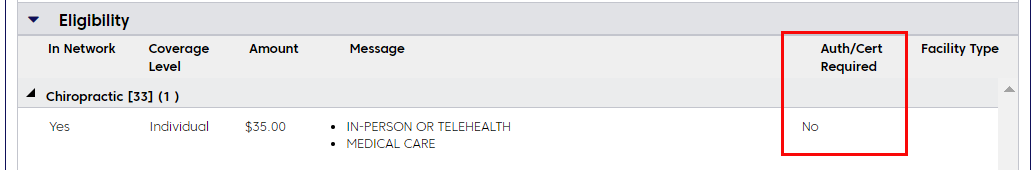
Request continued review before the member's 13th visit. You can do this using WholeHealth Living’s web-based Rapid Response System.
Continued review requests must be submitted within seven days (+/-) from the date of the member’s 13th visit.
It’s helpful to have the following information ready to enter into the Rapid Response System (web or phone-based).
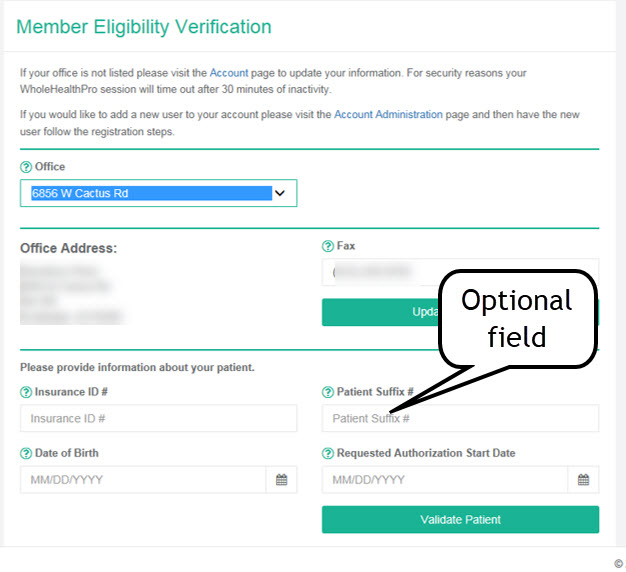
- The member’s ID number (prefix and suffix are not required) and date of birth.
- The injury mechanism (auto accident or work-related injury) or the presence of other insurance (if the other health insurance is primary and coordination of benefits applies).
- The member’s score from the Patient-specific Functional Scale (leave blank if member refuses to answer questions). The Patient-specific Functional Scale is available in English, Spanish, and Portuguese.
- Primary, secondary, and/or tertiary diagnosis codes.
You should also have the member’s medical record available since you will be asked multiple questions about the member’s diagnosis(es), medical history, and treatment plan.
Please refer to the Chiropractic Care Plan Authorization Request Form in the Appendix of the Chiropractic Services Authorization Program Guide for a complete list of the questions you will be asked to enter into the RRS.
- Web browser compatibility: Works best with Internet Explorer 11.
- Communication preferences: To get messages from WholeHealth Living about your requests, you’ll need to set up your communication preference. Choose either email or fax. You can change your preferences at any time.
- For email, we suggest using an email address that others in your office (who handle these requests) can access because an email can only go to one email address. When an email goes out about a review that has posted to the site, the email will be directed to that preferred email address. Then, you’ll need to log in to get the details about your patient.
- Message center: Your message center is your inbox. There, you’ll be able to read messages WholeHealth Living posts about your requests.
When a message is posted, you get an email. Please make sure your system is set up to receive emails from noreply@tivityhealth.com, so messages don’t go into your spam or junk folders.

If you receive an adverse determination and want to appeal the determination, you will have two options for reconsideration.
- Peer to Peer Requests: To request a discussion of the outcome of a clinical review with the peer reviewer who made the determination, please complete and return the "Request for a Peer to Peer Discussion" section of the UM Department Request Form. You’ll find more details on this process in the Chiropractic Services Authorization Program Guide.
- Appeal Requests: If you disagree with a medical necessity review outcome, you have the right to request an appeal. You’ll find more details on this process in the Chiropractic Services Authorization Program Guide.
To request an appeal for a pre-service or concurrent case:
- Please complete and return the UM Department Request Form. Be sure to fill out the "Provider request for a Reconsideration of a Medical Necessity Determination" section.
To request an appeal for a retrospective case:
- Please complete the UM Department Request Form and return it by fax or by mail using the address in your determination letter. Be sure to fill out the "Provider request for an Appeal of a Medical Necessity Determination" section.
WholeHealth Living’s dedicated support line: 1-866-656-6071
![]() Chiropractic Services Authorization Program Guide
Chiropractic Services Authorization Program Guide
![]() Frequently Asked Questions about the Program
Frequently Asked Questions about the Program
To download the Chiropractic payment policy, log in and click Find a Payment Policy on the right side of your home page. Or, go to Office Resources>Policies & Guidelines>Payment Policies.


