Habilitation services are health care services that help a person keep, learn, or improve skills and functioning for daily living.
Some members have outpatient benefits for habilitation care that are separate from their benefits for rehabilitation care.
For HMO members, authorization is required for these services.
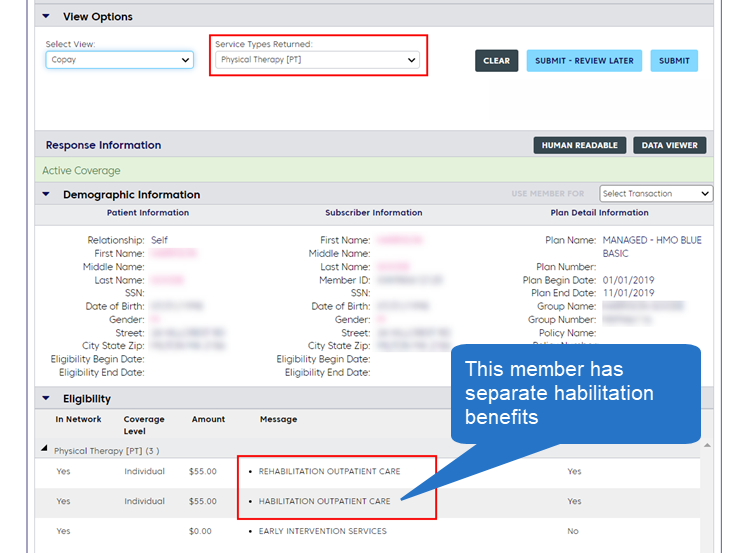
To determine if a member has separate habilitation benefits, perform an eligibility inquiry in ConnectCenterConnectCenter using the Service Type, "Physical Therapy" or "Occupational Therapy." When the member has separate benefits, the Message column in your results will list Rehabilitation and Habilitation separately as shown in the screenshot below.
To request an initial authorization for habilitation services, the PCP or authorized specialist should call Clinical Intake at 1‑800-327-6716. We'll work with you to get an authorization for up to 26 PT/OT (combined) visits in the current calendar year.
To request an extension of an existing authorization, the PCP or authorized specialist should fax us a completed Habilitative Therapy Request Form for HMO Members.
| If the member's benefits are | The PCP or authorized specialist can |
|---|---|
| Combined | Call Clinical Intake at 1-800-327-6716 to request an evaluation visit. Then, if additional visits are needed, we’ll need supporting documentation. Please follow the process for obtaining an outpatient rehab authorization extension for physical therapy or occupational therapy. |
| Separate | Use Authorization Manager to enter an authorization for an initial 26 PT/OT (combined) visits. The authorization period is the current calendar year. |
| If the member's benefits are | The PCP or authorized specialist can |
|---|---|
| Combined | Call Clinical Intake at 1-800-327-6716 to request an evaluation visit. Then, if additional visits are needed, we’ll need supporting documentation. Please fax us a completed Habilitative Therapy Request Form for HMO Members. |
| Separate | Call 1-800-327-6716 to request an authorization for an initial 26 PT/OT (combined) visits. The authorization period is the current calendar year. |
Occupational therapy (OT) and physical therapy (PT) services are typically a combined benefit under a member's short-term rehabilitation therapy benefits. Authorization is required for members in the following plans:
- HMO
- POS
- Medicare HMO Blue
- All occupational therapists employed by a group practice must contract with us.
- Authorizations to a occupational therapy group cover only contracted providers. Non-contracted occupational therapists can’t render services to a member, even if an authorization is granted to the group provider NPI.
Reminder: Benefits and benefit limits may vary by account. As always, please check the member’s benefits and eligibility before rendering services.
| For these members | You can request | Within this time period |
|---|---|---|
| Commercial HMO/POS plans | Up to 26 PT and up to 26 OT visits per provider | Per calendar year. |
| Medicare HMO Blue | Up to 12 visits each for PT and OT | Per 365-day authorization period. |
When a patient needs occupational or physical therapy, the member’s primary care provider (PCP) or an authorized specialist is responsible for requesting initial authorization for combined PT/OT visits. (Note: For Medicare Advantage members, only the PCP may submit outpatient rehabilitation therapy authorization requests.)
To do this, the PCP or specialist will need to use a technology. Be sure that you enter the appropriate group PT/OT NPI number. If the member’s maximum visits have already been met for the authorization period, a message will be displayed.
When the request is made electronically, we will automatically approve the initial visits. All authorizations processed in the current authorization period will have the same end date as the initial authorization.
Technologies you can use to submit your request
No authorization is required for members of the Federal Employee Program. However, benefit limits apply for Physical Therapy, Occupational Therapy and Speech Therapy combined.
| If | Then |
|---|---|
| The therapist determines that care beyond the initial visits is needed |
Important:
|
| The member has a new episode of care with the same provider within the same authorization period and the first visits have been used | A new initial evaluation is needed.
The authorization decision will be based on medical necessity criteria. |
To learn the status of an authorization, you can:
- Use an electronic technology like Authorization Manager.
- Enroll in our Automated Fax-back Program to receive daily notices of all service approvals and denials entered into our medical management authorization system for your facility/practice. Enrolled providers receive a Daily Inpatient and Outpatient Notification Report via fax.
For all members except Medicare HMO Blue:
To make medical necessity decisions for initial authorization and extension requests, we use InterQual® Criteria and our medical policies, as described in the subscriber certificate. Visit our InterQual Criteria() page for information about how to access these criteria.
For Medicare HMO Blue members:
We use Centers for Medicare & Medicaid Services (CMS) criteria. Please see the Medicare Benefit Policy Manual.
Primary care providers (PCPs) and designated specialists with an open referral from the PCP can refer a member for short-term rehabilitation therapies, including:
Physical therapy
Occupational therapy
Speech therapy
Habilitation Services
In most instances, the benefit for Massachusetts managed care group members is 60 visits per member per calendar year. The 60-visit maximum combines benefits for physical therapy (PT) and occupational therapy (OT) services. Speech therapy (ST) benefits are generally not included in the combined PT/OT short-term rehabilitation benefit. However, some self-funded accounts do combine the three therapies into one benefit.*
As always, it’s important for you to verify member benefits and eligibility before performing services.
*The short-term rehabilitation visit limit for Preferred Blue PPO® and Preferred Blue PPO Basic Saver® is 60 visits. The 60-day outpatient rehabilitation benefit limit does not apply to Medicare HMO Blue.
Occupational therapy (OT) and physical therapy (PT) services are typically a combined benefit under a member's short-term rehabilitation therapy benefits. Authorization is required for members in the following plans:
- HMO
- POS
- Medicare HMO Blue
- All physical therapists employed by a group practice must contract with us.
- Authorizations to a physical therapy group cover only contracted providers. Non-contracted physical therapists can’t render services to a member, even if an authorization is granted to the group provider NPI.
Reminder: Benefits and benefit limits may vary by account. As always, please check the member’s benefits and eligibility before rendering services.
| For these members | You can request | Within this time period |
|---|---|---|
| Commercial HMO/POS | Up to 26 PT visits and up to 26 OT visits per provider | Per calendar year. |
| Medicare HMO Blue | Up to 12 visits each for PT and OT | Per 365-day authorization period. |
When a patient needs physical or occupational therapy, the member’s primary care provider (PCP) or an authorized specialist is responsible for requesting initial authorization for combined PT/OT visits. (Note: For Medicare Advantage members, only the PCP may submit outpatient rehabilitation therapy authorization requests.)
To do this, the PCP or specialist will need to use a technology. Be sure that you enter the appropriate group PT/OT NPI number. If the member’s maximum visits have already been met for the authorization period, a message will be displayed.
When the request is made electronically, we will automatically approve the initial visits. All authorizations processed in the current authorization period will have the same end date as the initial authorization.
Technologies you can use to submit your request
- Authorization Manager. Follow the instructions in our Quick Tip and User Guide.
- Direct Connection.
No authorization is required for members of the Federal Employee Program. However, benefit limits apply for Physical Therapy, Occupational Therapy and Speech Therapy combined.
| If | Then |
|---|---|
| The therapist determines that care beyond the initial visits is needed |
Important:
|
| The member has a new episode of care with the same provider within the same authorization period and the first visits have been used | A new initial evaluation is needed.
The authorization decision will be based on medical necessity criteria. |
To learn the status of an authorization, you can:
- Use an electronic technology like Authorization Manager.
- Enroll in our Automated Fax-back Program to receive daily notices of all service approvals and denials entered into our medical management authorization system for your facility/practice. Enrolled providers receive a Daily Inpatient and Outpatient Notification Report via fax.
For all members except Medicare HMO Blue:
To make medical necessity decisions for initial authorization and extension requests, we use InterQual® Criteria and our medical policies, as described in the subscriber certificate. Visit our InterQual Criteria() page for information about how to access these criteria.
For Medicare HMO Blue members:
We use Centers for Medicare & Medicaid Services (CMS) criteria. Please see the Medicare Benefit Policy Manual.
Speech therapy services can sometimes be a combined benefit under an HMO/POS member’s short-term rehabilitation therapy benefits. For members of our Medicare HMO Blue Plan only, we require authorization for the initial 30 visits.
- All speech therapists employed by a group practice must contract with us.
- Authorizations to a speech therapy group cover only contracted providers. Non-contracted speech therapists can’t render services to a member, even if an authorization is granted to the group provider NPI.
When a patient needs speech therapy, their primary care provider (PCP) or an authorized specialist is responsible for generating an auto-approved initial authorization for the first 30 visits, every 365 days.
To do this, the PCP or specialist will need to use a technology. If the member’s maximum visits have already been met for the 365-day authorization period, a message will be displayed.
Technologies you can use to submit your request
No authorization is required for members of the Federal Employee Program. However, benefit limits apply for Physical Therapy, Occupational Therapy and Speech Therapy combined.
| If | Then |
|---|---|
| The speech therapist determines that care beyond the initial 30 visits is needed |
|
| The member has a new episode of care within the same 365-day period and the first 30 visits have been used |
The authorization decision will be based on medical necessity criteria. |
To learn the status of an authorization, you can:
- Use an electronic technology like Authorization Manager.
- Enroll in our Automated Fax-back Program to receive daily notices of all service approvals and denials entered into our medical management authorization system for your facility/practice. Enrolled providers receive a Daily Inpatient and Outpatient Notification Report via fax.
We use Centers for Medicare & Medicaid Services (CMS) criteria. Please refer to the Medicare Benefit Policy Manual.