This article is for all providers and their office staff submitting specialist referrals for their patients
As of November 1, 2021, providers can enter outpatient specialist referrals for members of our managed care plans using Authorization Manager.
- Primary care providers can enter specialist referrals, including for fertility services and oral surgery consults.
- Fertility/Assisted Reproductive Technology (ART) specialists can enter referrals for early pregnancy monitoring (EPM).
The ability to submit referrals is the latest feature we’ve added to Authorization Manager since launching the tool in February 2021. This allows users to enter all inpatient and outpatient authorization requests (service requests) and specialist referrals in one location, 24 hours a day, 7 days a week.
Entering referrals via Authorization Manager is simple
Instructions and a video demonstration of how to submit a referral are below. If you need to refer a member to a non-participating Blue Cross Blue Shield of Massachusetts provider, you must complete and return a Managed Care Out-of-Network Request Form.
How to enter a referral in Authorization Manager
Begin by following the process you use for requesting an authorization: enter Authorization Manager and click “Request Medical PA” on the left side of the screen.
The Request Medical Prior Authorizations screen will display. To enter a referral, select Outpatient Referral from the “Request Type” menu.
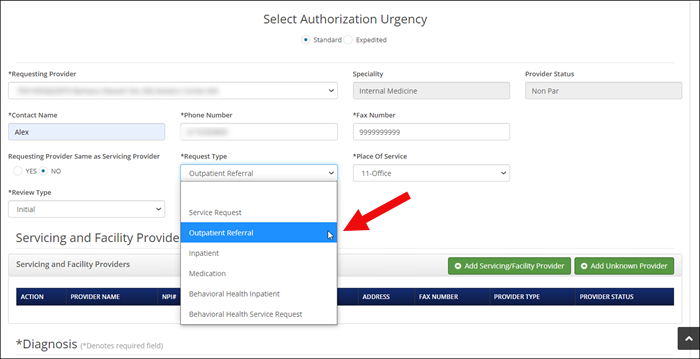
Select the appropriate options from the dropdown menus.
Important: Procedure code 99243 is required, as well as a diagnosis. If no diagnosis is available, you may enter general symptoms (R68.89).
Continue as you would with an authorization request.
When entering medical and behavioral health inpatient authorization requests
When building an authorization request, you need to check the priority type. For inpatient and behavioral health inpatient requests for members of the plans listed below, please choose priority type “Expedited” to ensure your case processes quickly.
| For plan types | For these plans, if you enter request type | And review type | With priority of | Instead, use priority of |
|---|---|---|---|---|
|
Commercial, New England Health Plan Host, Medex®', FEP |
Inpatient and behavioral health inpatient | Admitted | Standard | Expedited |
Resources
For more information visit our Authorization Manager page and click on Resources for tips and information about specific specialties or services.
- Video demonstration of how to submit a referral (for specialists)
- Video demonstration of how to submit a referral (for early pregnancy monitoring)
- Authorization Manager Guide (updated); see the section, “Entering authorization requests and referrals”
- Tips for Specialist Referrals
- Tips for Fertility Services/Assisted Reproductive Technology (ART) providers (revised)
- Managed Care Out-of-Network form
- Referrals Overview page, for a list of services that don’t require a referral
Questions?
For a live demo of Authorization Manager, please send an email to HMMAuthorizationManager@bcbsma.com.
MPC_012618-1L-78