You can manage referrals electronically using Authorization Manager, ConnectCenter, or a Direct Connection. Learn more about our technologies.
Note: A referral does not guarantee reimbursement. Member benefits and medical and payment policies may affect coverage and reimbursement.
Entering referrals
You can use eTools to enter and check referrals for all members in managed care plans, including those out of area. Referrals can be entered for up to 99 visits, and are good for 365 days.
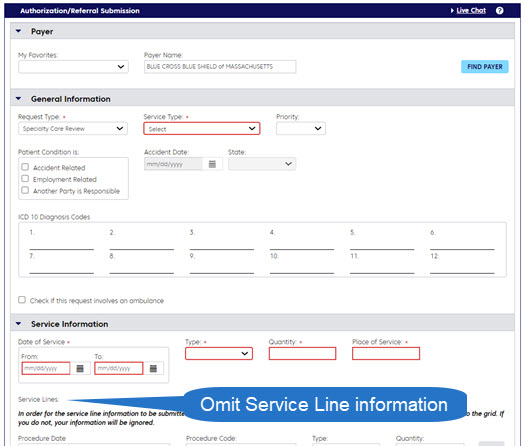
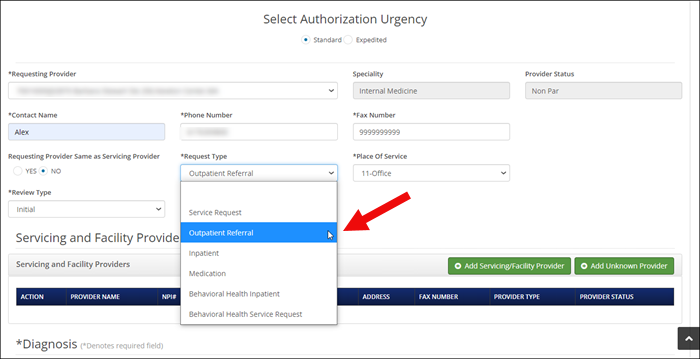
Important note for Authorization Manager: Procedure code 99243 is required, as well as a diagnosis. If no diagnosis is available, you may enter general symptoms (R68.89). Then continue as you would with an authorization request.
Verify referrals before rendering services
Verifying that a referral is on file and that the number of requested visits matches the services required helps facilitate the claims process and avoids unnecessary appeals or inquiries.
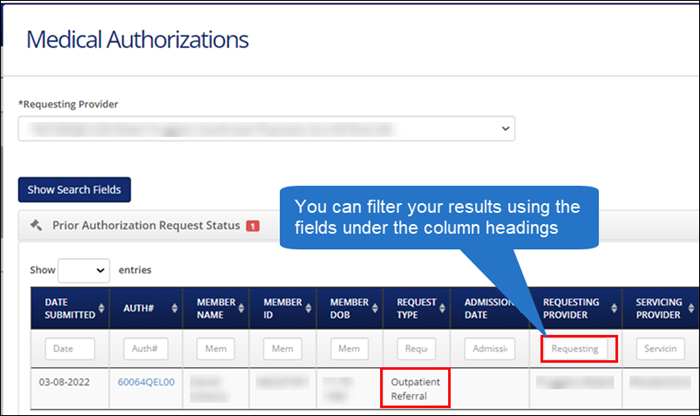
To search for an existing referral in Authorization Manager go to the View Authorizations screen. You can filter your list by typing "referral" under the column heading, Request Type.
With Authorization Manager, you can see both the Requesting Provider and the Servicing Provider.
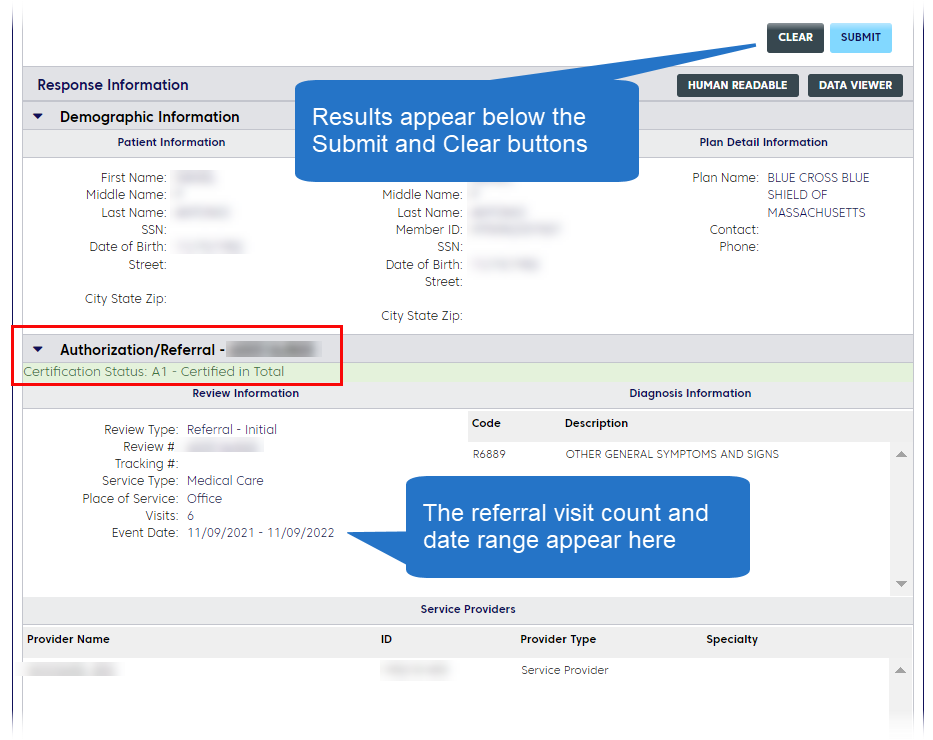
To verify a referral in ConnectCenter, go to Verification> Authorization/Referral Status. Complete the required fields and click Submit.
- For Provider Type, select "Specialist" for any individual provider (non-facility).
If a referral is active, your results will look like this: