The New England Health Plans (NEHP) offer employers a regional managed care benefit plan that covers all employees regardless of where they live or work in New England.
Participating Blue Cross Blue Shield Plans include:
| Home/Host Plans |
|
|---|---|
| Home Plan only |
|
As with the larger BlueCard program, the Blue Cross Blue Shield Plan that the member has enrolled in is called their Home plan. The member’s benefits are determined by their Home Plan.
In general, when a member receives services outside of their Home Plan area, the Plan in the area where they receive services is called the Host Plan. Host Plans route electronic transactions to the member’s Home Plan for processing.
New England Health Plan members can select a primary care provider (PCP) in any of the six New England states. Whether an authorization is required for medical or surgical care is determined by the area where the member’s PCP is located. (Behavioral health care is the exception; referrals and authorization requests for these services should be sent to the member’s Home Plan.)
Blue Cross Blue Shield of Massachusetts offers HMO and POS plan designs through these five products:
HMO
- HMO Blue New England
- Network Blue New England®
- Access Blue New England
POS
- Blue Choice New England®
- Blue Choice II New England®
HMO Blue New England plans require a primary care provider (PCP) for the coordination of the member's care and for referrals to an in-network specialist.
Blue Choice New England plans require a PCP for the coordination of the members care, but provides the member the flexibility to self-refer to any BCBS-participating provider.
Access Blue New England plans require a PCP for the coordination of the members care, but provides the member the flexibility to self-refer to specialists within the network.
You can identify NEHP members by their Blue Cross Blue Shield ID card. Be sure to ask all visiting members for their ID card. The main identifier for NEHP Plans is the name of the health plan/product in the upper right-hand corner of the ID card, and the three-character prefix preceding the ID. You’ll also see the suitcase logo on the card. Identifying members from other states is easy. Below we’ve listed the ID card prefixes for each state offering plans. Members from other states may be entitled to additional mandated benefits.
| State | Prefix |
|---|---|
| Connecticut | CTN, CTP, EHF, APQ, APR, APG |
| Maine | MEN, MEP, EHG, BFZ, BDD, BHI, XJV, MEY, TXH |
| New Hampshire | NHN, NHP, EHH, BKA, NMY, BYV, YGI, BPP, YGE, ZZG, YGL, ZXW |
| Rhode Island | RIN, RIS, RIA |
Primary care providers: For NEHP members, submit referrals to the local plan (that is, the plan in the state where you’re located).
Visit our Referrals page for more information about which services require a referral.
Authorization requirements are determined by the state where a NEHP member’s PCP is located.
- For members with Massachusetts-based PCPs, refer to our Prior Authorization Overview page for instructions.
- For members with PCPs in other states, refer to the local Plan’s website.
- Vermont: bluecrossvt.org/providers
- Anthem (CT, NH, ME): anthem.com/provider
- Rhode Island: bcbsri.com/providers
You can use ConnectCenter to learn the location of a member’s PCP.
Eligibility search results vary depending on the member’s plan and product, but the screenshot below shows an example for one member.
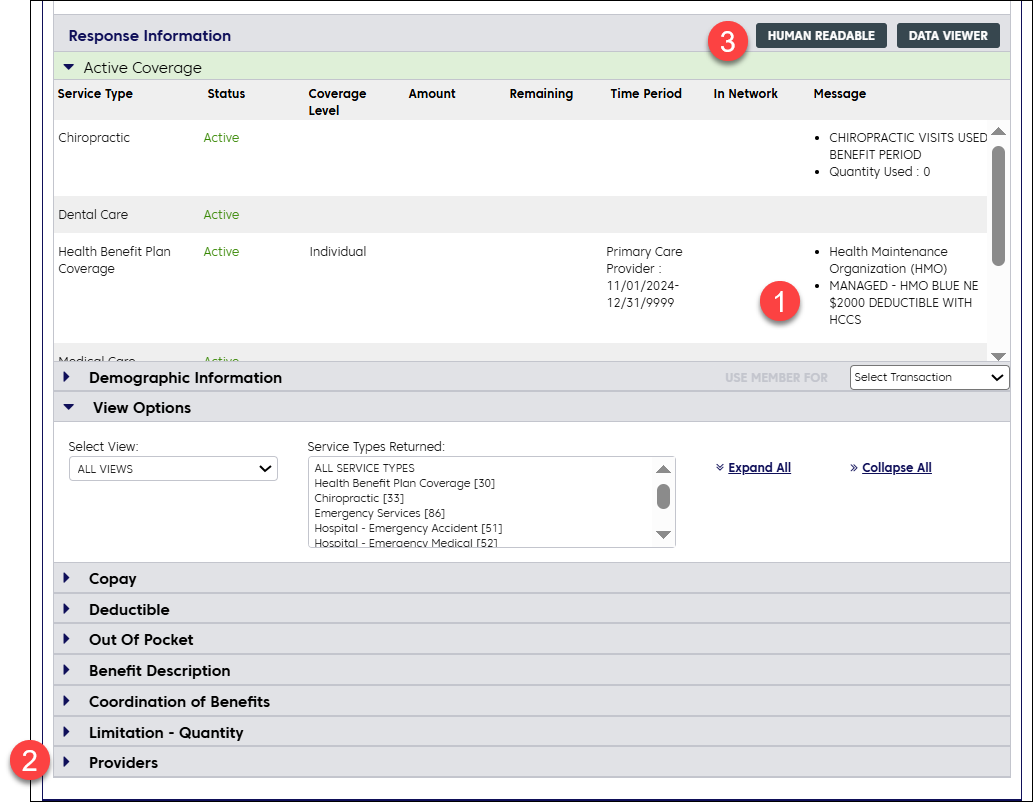
Follow these steps to learn about the member’s PCP:
- Perform an eligibility inquiry in ConnectCenter and verify the member’s plan and coverage status.
- Scroll to the “Providers” accordion at the bottom of your results and expand this area. If the member is a Massachusetts member and has a Massachusetts PCP, you will see the PCP’s contact information.
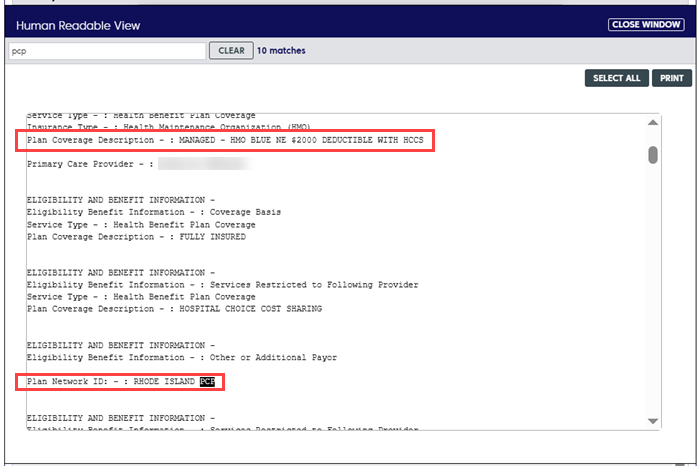
- If you don’t see contact information in the “Providers” area, click the button, “Human Readable.” This will open a window showing results directly from the member’s Blue Plan.
- When you open the Human Readable window, search for "pcp" and scroll to the highlighted text. The example below shows that the member has a Rhode Island PCP.